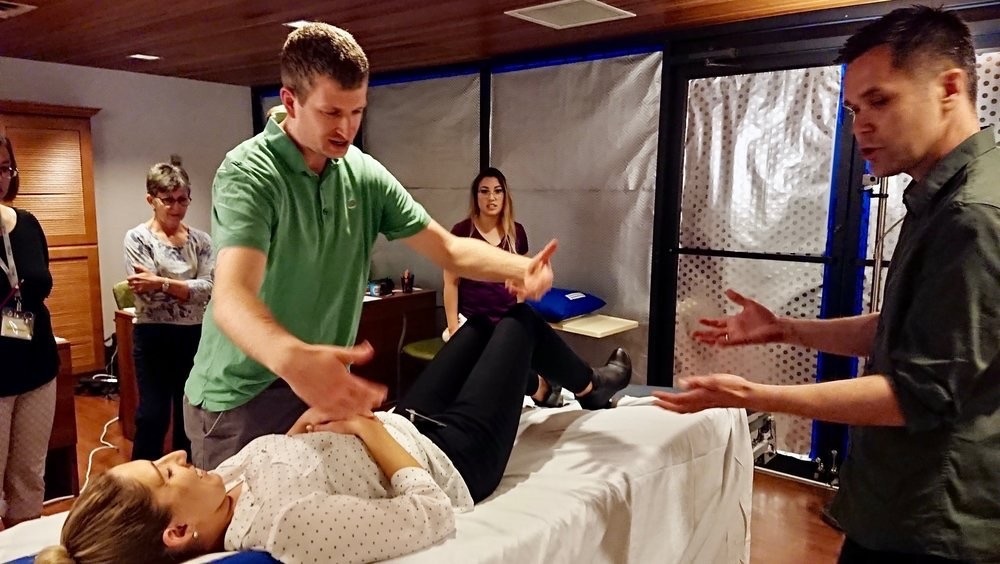
HHS GERAS co-designs a ‘smart’ hospital bed
Norwegian-based Ably Medical can rest easier, thanks to feedback from Hamilton Health Sciences on the world’s first ‘smart’ hospital bed, developed by the Scandinavian company.
The Ably Bed was designed to assist caregivers as well as patients, since its technology is intended to help prevent pressure ulcers and falls, and help reduce injuries to nursing staff by making it easier to safely maneuver patients in their beds.
Ably in partnership with HHS GERAS Centre for Aging Research led the research study to pilot the bed and assess its impact on patient care and the work of health care providers. HHS staff, management and leadership provided feedback on the initial prototype as well as a modified version.
HHS leads pilot project
“Amazing to watch”
“It was amazing to watch the dedicated staff at HHS engage in the design thinking process to modify and improve the Ably prototype bed,” said George Ioannidis, associate scientific director for GERAS. “The staff’s enthusiasm and excitement for the co-design method ensure that the Ably Bed meets the needs of frontline care professionals and their patients.”
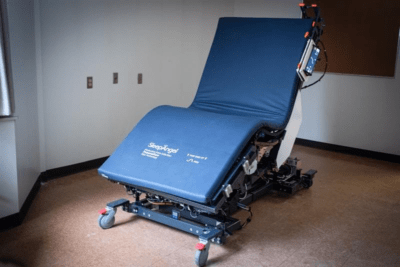
In 2018, staff, management and leadership spent four weeks testing the initial prototype bed at HHS St. Peter’s Hospital and provided feedback to Ably. Recommendations included suggestions about the placement and design of a control panel since the prototype didn’t have one. Nurses also suggested that it have the ability to go lower, so it would be easier to maneuver patients safely.
In November 2019, the new and improved prototype bed arrived at St. Peter’s for a three-week trial. Patients were not part of either pilot, however the next phase of the study would see the bed used in patient care.
Ably Bed technology includes machine learning
“The Ably partnership is testimony to GERAS’s leadership in research and innovation.”
The Ably Bed combines a groundbreaking movement system as well as a range of sensors that monitor and improve the comfort of the patient while reducing workload of clinical staff.
“Partnering our talented scientific investigators with exciting, innovative companies is key to designing solutions that work for our patients and staff,” said Ted Scott, Vice President of Research and Chief Innovation Officer for HHS. “The Ably partnership is testimony to GERAS’s leadership in research and innovation.”
Ably’s ‘smart’ bed frame consists of motion springs that allow for new movement possibilities, supporting patient treatment and healthcare workers in their everyday work, including lifting and moving patients. This wireless bed has sensors built in that allow for continuous vital sign monitoring of patients including heart rate, breathing rates, weight and movement patterns.
Patient data may be available either at the bedside, the nurse’s station or directly to handheld devices. When patient data changes, the system predicts possible outcomes and provides insights the health care team can use for early intervention.
In addition, the bed’s design models the human spine and moves to provide better mobility and stability. Finally, using data from the monitoring system and bed frame, the bed is capable of machine learning and is able to learn to react proactively to patients to avoid critical situations.
Validating design and function
Over the past two years, GERAS, HHS and the Ably medical team worked with nurses and other clinical staff who perform patient handling tasks including doctors, occupational therapists and physiotherapists. User feedback has enabled ABLY to validate the concept, optimize and improve the technology of the bed, making modifications as necessary.
Funding for the 24-month project was secured by Ably Medical and four hospitals in Ontario (HHS, West Park Health Centre in Toronto, Southlake Regional Health Centre in Newmarket and Mackenzie Health in Richmond Hill) through the Toronto-based Centre for Aging + Brain Health Innovation and its Industry Innovation Partnership Program.
Next steps
The next phase of research will include patient trials to determine if the technology improves pressure ulcer prevention and fall prevention, as well as reducing the physical and mental nurse burden in a hospital setting. Further studies and health economics analysis are required to specify actual cost savings/cost effectiveness to healthcare systems.
Related:
https://www.gerascentre.ca/baycrest-cabhi-12p2-ably-bed-project/
