
Designated COVID units make time for compassion
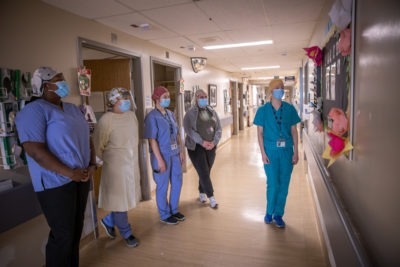
It doesn’t look all that different from a standard hospital unit. Staff are calm, coordinated. They move around one another in a well-choreographed dance as they care for patients, check test results, and disinfect surfaces. But a trained eye will notice some important distinctions—layers of PPE including face shields, gloves, and gowns are applied before interacting with patients. Signage politely warns that rooms should only be entered for essential care. And the hallway near the entrance and exit is decked with two colourful bulletin boards: one honouring the people who didn’t make it, and one celebrating those who did.
Amazing care
 Beverly Blackwood made her departure from Hamilton Health Sciences’ 8 West (HHS) COVID unit in May. The 69-year old was wheeled down the hall flanked by staff and doctors cheering her on after 40 long days on the unit.
Beverly Blackwood made her departure from Hamilton Health Sciences’ 8 West (HHS) COVID unit in May. The 69-year old was wheeled down the hall flanked by staff and doctors cheering her on after 40 long days on the unit.
She came to the hospital after an outbreak in the care home where she was staying and remained for several weeks. She barely recalls her trip to the hospital. Following her positive test result, she says everything was a blur for the first week or so. “They told me for the first week I was crying out for help, and not wanting to eat.”
Focused on the silver lining, Blackwood says that her diagnosis was traumatic, but she was very glad to have ended up at HHS’ Hamilton General Hospital.
“The care I got here was amazing,” she says. “It’s upsetting to have this sickness, but when you have people who care, checking in on you, cleaning the room twice a day, you feel so cared for.”
It takes a special blend of compassion and courage to work on a COVID unit. Both 8 West and ICU South at HGH are devoted to COVID patients. They are grouped together to prevent the disease from spreading into other areas of the hospital. The staff and doctors on these units know they are coming to work every day in an environment where the virus exists.
Dedicated team
“We’ve been very fortunate to empty out the one floor and maintain one dedicated space to caring for these patients and one dedicated group of individuals to care for them,” says registered nurse Corry Koning. “With us being the designated unit we can really understand what we need to do to care for them and how best to care for them.”
Staff and doctors take extreme care to protect both their patients and themselves. The ritual ‘donning and doffing’ of PPE is exact. Environmental aides methodically clean every possible surface that has been touched. These additional measures can add to the workload and stress of the job, but the team finds time for little personal moments with patients, even in the ICU.
Tender moments
 “I feel my colleagues have truly stepped up,” says Claudia Poulin, a charge respiratory therapist. “To hold hands when people are short of breath, or to assure patients that they are safe when in isolation rooms. I think this virus has strengthened our talent to roll with the punches and adapt to uncharted waters.”
“I feel my colleagues have truly stepped up,” says Claudia Poulin, a charge respiratory therapist. “To hold hands when people are short of breath, or to assure patients that they are safe when in isolation rooms. I think this virus has strengthened our talent to roll with the punches and adapt to uncharted waters.”
Those tender moments made a lasting impression on Blackwood. She says she has many warm memories from this otherwise terrifying time. “It made me feel special. I certainly didn’t feel special when I came in here. I thought I was dying.”
“We have never been too overwhelmed or short-staffed to provide the compassion, respect and empathy these people deserve when hospitalized during this pandemic,” adds Poulin.
All staff caring for COVID patients agree that the experience has brought them closer together. They have drawn on each other’s courage, skills, and kindness to deliver the best possible care.
