
‘Dia-besties’ manage their type 1 diabetes together
Like most kindergarten kids, classmates Julia and Ainsley were learning their ABCs and 123s. But the five-year-old girls were also introduced to the world of science and nutrition at this very young age, after being diagnosed one week apart with type 1 diabetes (T1D).
T1D is an autoimmune insulin deficiency that prevents the body from producing insulin on its own, or very little of it. Insulin is a hormone that helps your body turn food into energy, and regulate blood sugar levels. An individual with T1D must intake insulin via injection or insulin pump in order to survive.
Working with their parents and McMaster Children’s Hospital (MCH) health-care teams, the girls — now 11 years old and good friends — have learned how to keep on top of their sugar levels, calculate carbohydrates, and give themselves insulin. When it comes to managing their disease, they love the support of having a ‘dia-bestie’ with the same diagnosis.
Diagnosed a week apart

Ainsley and Julia have quick access to their blood sugar tracking, an important part of diabetes management.
When Julia was five years old, she was losing weight and always very thirsty. After a visit to her family doctor, test results showed she had high blood sugar, a sign of diabetes. Shortly after receiving care at MCH, she started feeling better.
When Ainsley was also five, she was so thirsty at night that she would wake up crying from discomfort. Her family doctor administered a simple urine test, and results immediately showed glucose in her urine; a sign of T1D. She was sent to MCH for further care.
“I called the school to let them know Ainsley’s situation and how she was going to be away for a few days, and they told me another parent made the same phone call shortly before me,” says Kate Adams, Ainsley’s mom.
The pair were diagnosed a week apart, and were both in the same junior kindergarten class at Spring Valley Elementary School in Ancaster. Shortly after, the two kids and their moms became close friends, embarking together on the same journey. Julia and Ainsley are still at the same school, now in Grade 6 but in different classes this year.
“It gives an incredible peace of mind to have someone who understands the day-to-day challenges. You problem solve together,” — Kate Adams, Ainsley’s mom.
How to manage T1D in children

Dr. Ereny Bassilious, pediatric endocrinologist at McMaster Children’s Hospital, works with both Julia and Ainsley.
Children with type 1 diabetes manage the disease with insulin that’s administered by injection or infused via insulin pump into the bloodstream continuously and increased before every meal and major snack. They need to check and monitor their blood sugar levels frequently as well to keep insulin and glucose balanced. This can be done through finger pokes or other new sensor technologies. High blood sugar can lead to a rapid heartbeat, vision problems and other symptoms. And too much insulin can lead to low blood sugar causing shakiness, disorientation or even loss of consciousness.
“They have to think about so many different things,” says Dr. Ereny Bassilious, a pediatric endocrinologist at MCH who works with both girls. “It is difficult as a young child with T1D because of the complexity of it. There are so many steps that go into managing diabetes such as checking sugar, counting carbohydrates, calculating insulin dose, and administering the insulin.”
Using technology to make life easier
A newer technology known as continuous glucose monitoring (CGM) happens through a device worn on the body that tracks blood glucose (sugar) levels every few minutes throughout the day and night. These readings are sent to the patient, caregiver, or health-care provider via a digital device for fast and accurate readings, minimizing the need for finger pokes.

Ainsley shows how her glucose monitor sends her blood sugar levels to her phone. They go to her mom’s phone as well.
Both Ainsley and Julia use a CGM system that tracks blood sugar levels and sends frequent readings to a paired smart device. It allows for both moms to also pair their phones to the device and monitor their daughters’ sugars while they are at school.
“CGM technology allows the patient and caregivers to monitor blood sugars continuously, to observe trends, and to be able to act on a high or low blood sugar in a timely way,” says Dr. Bassilious.
“A caregiver of a young active child with diabetes can make over 100 treatment decisions a day,” — Sarah Fairfield, Julia’s mom.
Instead of frequent needles, many young people may choose to use an insulin pump, which is a clear little tube that administers insulin to the body when told to, and is attached to them at all times.
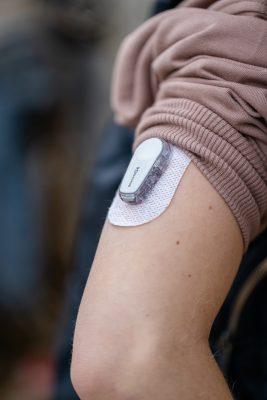
Both girls use a sensor to continuously track glucose levels.
For their insulin, both Ainsley and Julia use a pump, eliminating the need for multiple daily injections. Base insulin deliveries are programmed into the pump by their health care team. Insulin delivery for meals or for correction of high blood sugars is delivered when the child or their caregiver enters a blood sugar or carb amount into the pump.
“There are lots of elements involved in diabetes management,” says Bassilious. “With young children, we strongly recommend a partnership between health-care providers and parents, before slowly transitioning over to the child doing things on their own.”
MCH cares for about 665 young patients with diabetes. Along with a treating physician, there is a whole team that helps families with learning about the disease and how to manage it. The team consists of a diabetes nurse, dietitian, child life specialist, and social worker.
A confidant, mother, and friend
“As a parent, you are overwhelmed at first,” says Sarah Fairfield, Julia’s mom. “It’s a whole new routine, a new lifestyle. There is a lot to learn in the beginning. A caregiver of a young active child with diabetes can make over 100 treatment decisions a day. There is so much planning that goes into it.”
As much as the girls find support in each other, their moms also have comfort in knowing that their daughter’s friend has a family who knows how to handle their health needs.
“Things like sleepovers can be tricky,” says Adams. “You have to know a little bit of what is going on. As the mom, you can only plan so much with packing snacks and everything else. When Ainsley goes to Julia’s for a sleepover, I know I don’t have to worry.”
Fairfield adds, “It gives an incredible peace of mind to have someone who understands the day-to-day challenges. You problem solve together.”
The “Golden Unicorn” friendship

The girls demonstrating their gymnastics moves. Both girls manage the impact of their favourite physical activities with their diabetes.
Ainsley and Julia are the only students in their grade at their school with T1D.
“Whenever our levels would match up, we used to make jokes about how we were golden unicorns,” says Julia.
Ainsley adds, “If I ever needed anything I can go to Julia. If I need something like Dextabs at school I would be able to ask her for some. I remember one day at school, I saw Julia a little shaky and I ran over right away because I knew the signs of what was happening.” Ainsley is referring to a situation where she noticed Julia was experiencing signs of low blood sugar levels.
Both girls attend Diabetes Canada Camp every summer, along with Bassilious, a camp doctor, who is referred to as one of their “camp buddies.”
“The biggest thing is making sure children remain children throughout all of it,” says Bassilious. “They have such a resilient spirit, and the partnership with their mothers in managing their diabetes is extremely incredible.”
Adams agrees. “I think they are both amazing examples of kids who are thriving despite what they have to do on a daily basis.”
“It doesn’t define you.”
“Kids still need to be kids,” says Bassilious. “They need to eat in order to grow, and do all the things they enjoy. Diabetes is manageable – it doesn’t define who they are.”
Ainsley is a competitive dancer who does jazz, lyrical, hip-hop, contemporary, tap, and ballet. She plans ahead to manage her sugars on long dance nights.
“I have to keep on top of it. You can still do all of your activities and eat, just make sure you plan, monitor, dose and don’t let it hold you back,” says Ainsley.
When Julia isn’t bike riding or getting her favourite slushies, she is a talented gymnast. She doesn’t let diabetes get in the way of her jumps, flips, and twists.
Both parents express the importance of breaking the stigma of stereotypes around T1D.
“You hear so many stereotypes about diabetes – people think it’s because you don’t eat healthy or you’re not active,” says Adams. “That is not the truth at all.”
“The biggest thing is making sure children remain children throughout all of it,” says Bassilious. “Whether it be trick-or-treating or having pizza and cake at a birthday party or playing their favorite sport, it is important children and youth living with T1D continue to do what they enjoy.”



