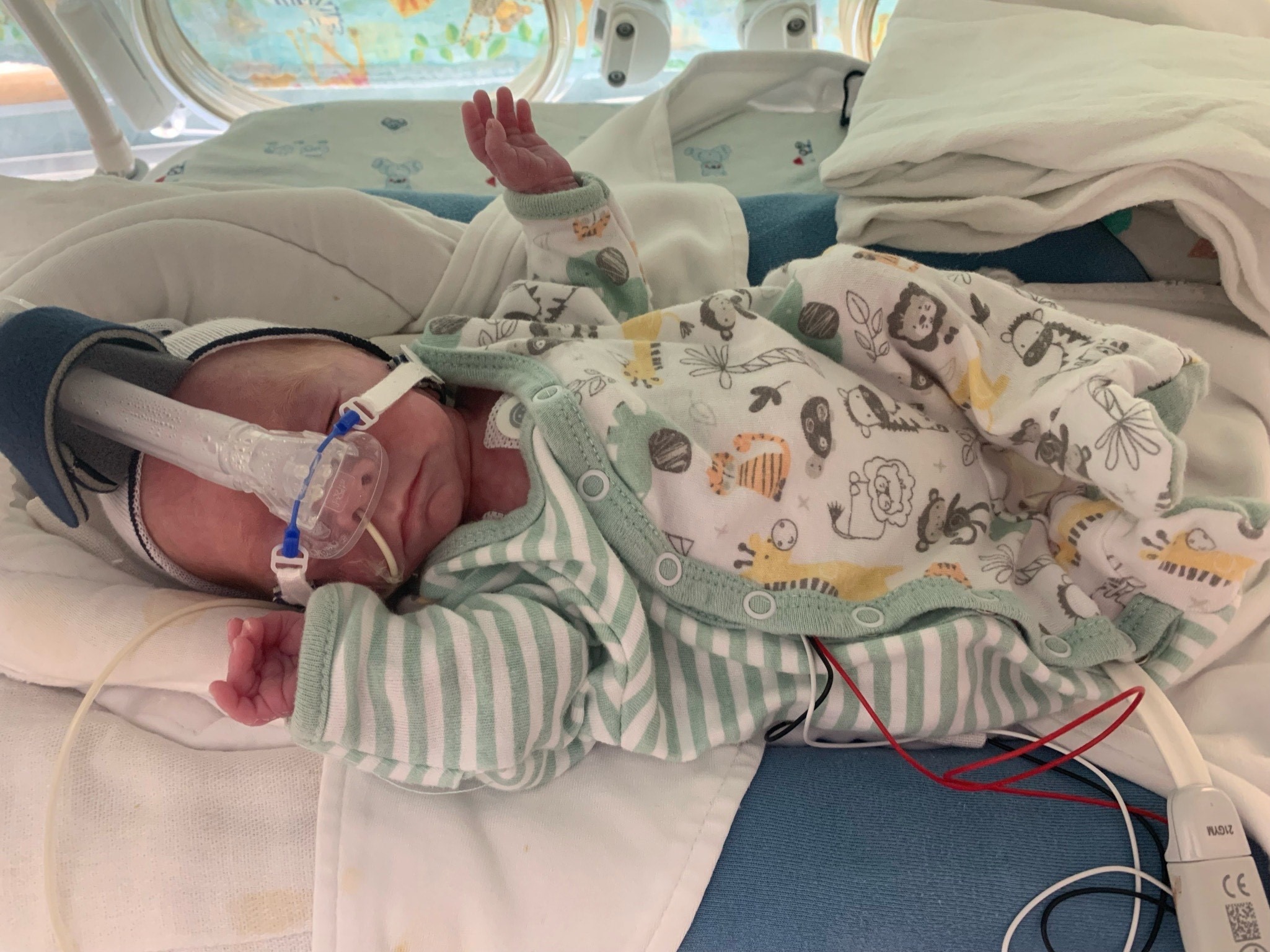
First-time parents overcome challenges in NICU
On May 4, baby Luca came into the world a little earlier than expected, weighing just over one pound. Facing various health issues, Luca is still receiving care in the Neonatal Intensive Care Unit (NICU) at Hamilton Health Sciences’ McMaster Children’s Hospital (MCH).
Early in his stay, his mom Krista also found herself facing health hurdles of her own and received care at Hamilton Health Sciences’ Hamilton General Hospital until she could rejoin Luca.
A delivery plan in place
At 20 weeks into her pregnancy, Krista was referred to the Maternal-Fetal Medicine unit at MCH because Luca’s size was significantly below average for his stage of development. “At this point, we knew Luca would need to be delivered via C-section at Mac and would likely have a lengthy stay in the NICU,” says Krista. She also had a series of complications that required her to be closely monitored to track Luca’s growth.
Just shy of the 30-week mark in her pregnancy, Krista was admitted to the labour and delivery department at MCH for closer monitoring, as Luca’s heart rate was dropping and showing signs of stress. A few days later, Luca was delivered via C-section weighing just 475g. Most babies arrive between 39 and 42 weeks of pregnancy and can be anywhere between 3-4kg when they are born.
Overwhelming NICU journey

Krista and Luca both faced health challenges simultaneously, but have been doing well.
Luca has been a NICU patient since birth. “As first-time parents, we were incredibly overwhelmed,” says Krista. “We would do anything to help our little boy and it was very difficult those first few weeks seeing him in his incubator with many wires and tubes attached to him. At times we felt helpless, but we knew he was safe and cared for in the NICU.”
Unfortunately, Luca developed some health issues at just a couple of days old. He experienced a serious infection, and had very small lungs at birth, which presented further health challenges down the road.
Understanding a tracheostomy

A smiling, thriving trach baby.
In late August, his medical team discussed the possibility of re-intubating or performing a tracheostomy on Luca. This was due to his increased respiratory needs while on CPAP, which is a ventilation system that uses mild air pressure to keep breathing airways open and his lungs inflated.
A tracheostomy involves inserting a tube in the neck to assist with breathing.
“At the same time, I was admitted to Hamilton General for two weeks for pancreatitis and gallstones,” says Krista. “During these two weeks, Luca’s respiratory needs continued to increase and they were starting to see early signs of pulmonary hypertension.” Pulmonary hypertension is a condition that affects the blood vessels in the lungs.
Luca’s parents discussed the complications with his doctors and a respiratory therapist. The health care team explained the benefits and risks of the tracheostomy. Krista’s husband, Eric, decided that a trach and g-tube were the best options for Luca’s health. The health care team then scheduled the procedures quickly.
“Luca’s biggest challenge was his respiratory status,” says Victoria Kranjac, one of Luca’s primary registered nurses. “He was on continuous respiratory support and still having difficulty with a high respiratory rate (fast breathing) and requiring oxygen. Due to this, his parents decided to go ahead with the tracheostomy to allow his lungs the time they needed to grow.”
Surgeries for both mom and baby
“In early September I had surgery to remove my gallbladder, and just a few days after that, Luca had his surgery,” says Krista.
Luca’s surgery went very well. “After a few weeks of recovery, our tired and grumpy CPAP baby became a smiley, energetic and thriving trach baby.”
When Luca underwent his tracheostomy, Michele English, a respiratory therapist, joined their NICU family. English provided Krista and Eric with training on how to care for Luca once he returned home.
Krista says she was impressed with English’s knowledge and expertise, which made her feel confident in responding to any emergency that may arise. “Throughout the process, Michele was a listening ear, a helping hand, and a reassuring presence for us. We’re incredibly grateful for all that she does to help little ones and their families, especially in the preparation for life outside of the NICU with a tracheostomy-dependent baby.”
A care team that feels like family
During Luca’s stay in the hospital, he’s been receiving care from various team members in the NICU. His primary nurse, Kranjac, has been with him since birth and plays a significant role in his care.
“I have been taking care of Luca since the beginning and will continue to do so until he’s discharged,” says Kranjac. “Working with Luca’s family has been an absolute dream. I feel fortunate to be able to work with him and his family whenever I’m at work. I am grateful to have witnessed his growth over the months and see him transform into the adorable little man he is today.”
Krista says, “We are extremely thankful for all the kind and thoughtful things Victoria has done for Luca and us during this time. Her efforts have helped us feel comfortable and well-cared for.”

Victoria Kranjac and Tim Buxbaum pictured with Luca, feeling festive in the NICU.
Due to Luca’s tracheostomy, he will require 24/7 care until his lungs are grown and healed enough to have the trach removed. In order for Krista and Eric to get some well-needed rest when they return home, they will need to have nurses who will come and provide care at home every night. Luckily, one of the nurses who will be caring for Luca at home after discharge will be Kranjac.
“We used to joke that we would need her to move in with us after we were discharged to help take care of Luca, and now we are thrilled that she will be part of our home-care team to help care for him when she isn’t in the NICU,” says Krista. Kranjac has been hired on privately as a home-care nurse to provide care for Luca when she is not working at the NICU. This has been made possible through the family-managed home-care program, and Home and Community Care services.
Kranjac mentions how “firsts” with Luca and his parents were some of the most memorable moments caring for Luca – opening his eyes, having skin-to-skin contact with his parents, first bath, and the first time he was free of IV fluids. “While some of these milestones may not seem significant to all parents, they are crucial in the journeys of our NICU patients,” says Kranjac.
Before Luca’s surgery in early September, the family was also overjoyed to welcome “Uncle” Tim Buxbaum to Luca’s team as another primary nurse. Krista says that Tim’s exceptional care for Luca coupled with his humor and joy has allowed her and her husband to laugh and smile, even on some of their most stressful and scary days. “Tim has become like family to us, and his attention and care have helped Luca to flourish and grow.”
A message of gratitude
Now seven months old, Luca is still in the NICU, but his family is excited for his planned discharge on February 1, 2024.
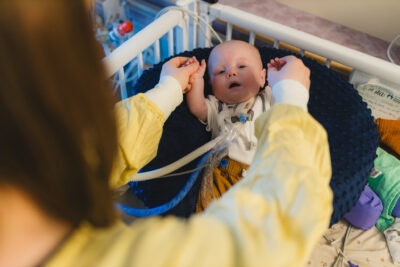
A big cheer for our NICU from Luca.
“The care that Luca has received in the NICU has been exceptional,” says Krista. “It made it easier for us as parents to take much-needed breaks for ourselves, knowing that he was in good hands and cared for by people who love him almost as much as we do.”
She adds that Luca loves to smile and interact with all the nurses, respiratory therapists, doctors, and support staff who visit him. “We’re thankful for all they do every day to help make our NICU home a safe space for Luca to grow.”