Introducing an Anesthesia Assistant
Aaron Walsh supports an expanding new role in adult surgical and perioperative care
Inspiration strikes in many ways, often when least expected. When Aaron Walsh was a teenager on a three-week wilderness trip, a chance encounter with a guide who was also a paramedic led him to pursue a career in healthcare, which eventually brought him to the anesthesia team at Hamilton Health Sciences (HHS).
After working as a land-based paramedic for two years, Walsh became a fight paramedic with Ornge, the provincial emergency air ambulance operator. This opened up additional areas of interest for him, and with the experience and skills he acquired as a paramedic, he decided to take another leap and completed a nursing degree at Brock University. For three years, Walsh provided bedside nursing care in the intensive care unit at Juravinski Hospital before pursuing his next goal of becoming an anesthesia assistant. Last year, he graduated from the Anesthesia Assistant Program at University Health Network’s (UHN) Michener Institute of Education.
Walsh now supports surgical and perioperative care at Juravinski Hospital, as one of two anesthesia assistants who are part of the site’s Anesthesia Care Team (ACT). In Canada, anesthesia assistants are registered nurses or registered respiratory therapists who have taken additional training to work in this unique field.
“Anesthesia assistants can be part of the solution.”
Solutions for safe patient care
Although the profession is relatively new in Canada, for a number of years, anesthesia assistants have been working away quietly at McMaster Children’s Hospital as part of the pediatric sedation team. Recently, however, the Department of Anesthesia started expanding the role to adult sites.
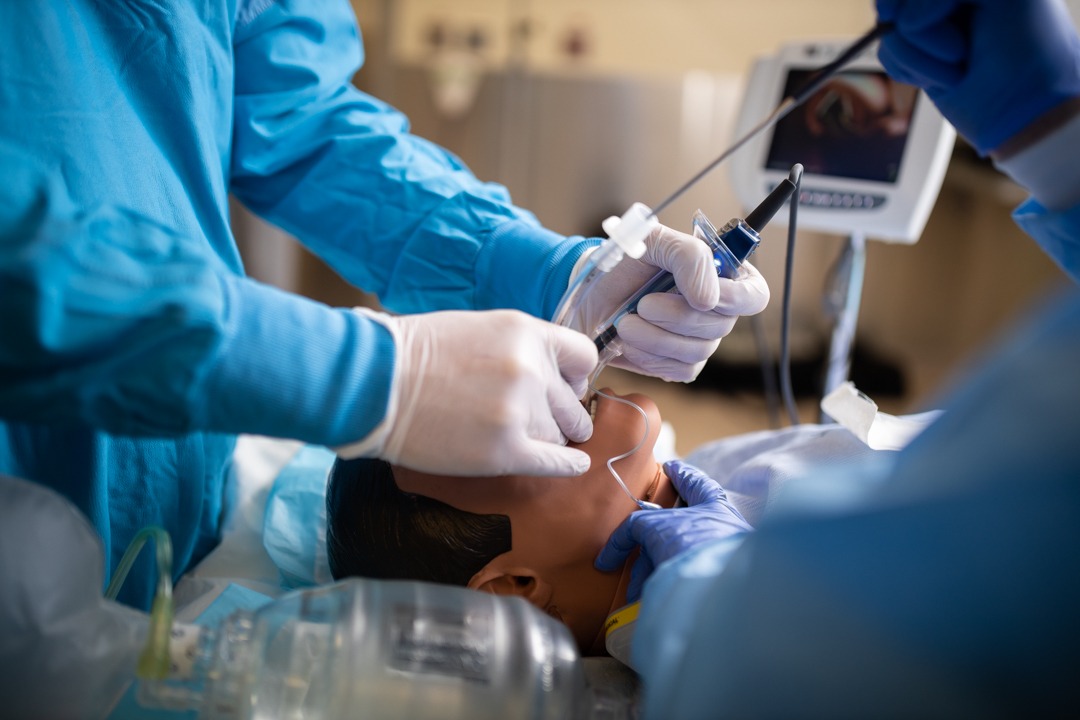
Anesthesia assistants provide support for attending anesthesiologists to help ensure that a patient is ‘anesthesia ready’ faster than if the anesthesiologist was working alone. During a typical procedure, Walsh provides start-up assistance before the patient can be prepared by the surgical team. This varies depending on the patient and the procedure, but may include giving medication to put the patient to sleep or to maintain blood pressure, administering of antibiotics, and placing monitors and inserting additional lines. Some patients under general anesthetic may require extra support for the placement of a breathing tube when it is challenging to secure their airway.
“This is a crucial step because the patient isn’t breathing on their own when the tube goes in, and there may be a period of time when the patient isn’t able to breathe at all,” says Walsh. Using his skills and special equipment, he helps to ensure a potentially dangerous situation is averted.
Rewarding role
For Walsh, depending on the types of surgical cases being performed, day-to-day responsibilities include working in conjunction with an operating room respiratory therapist and ensuring that anesthetic equipment and supplies are checked and ready for use.
“For the anesthesiologist, having an assistant who has received specific training in the specialty and can anticipate direction is extremely helpful in a crisis situation,” he says. “Even in the most routine cases, a skilled assistant is able to improve efficiency. Because of the latest COVID wave, we have a huge number of people waiting to get their surgeries. Anesthesia assistants can be part of the solution.”
There are a multitude of aspects to the role that Walsh finds rewarding, such as helping a patient understand their care plan, doing procedures, helping to teach students and working in a team environment.