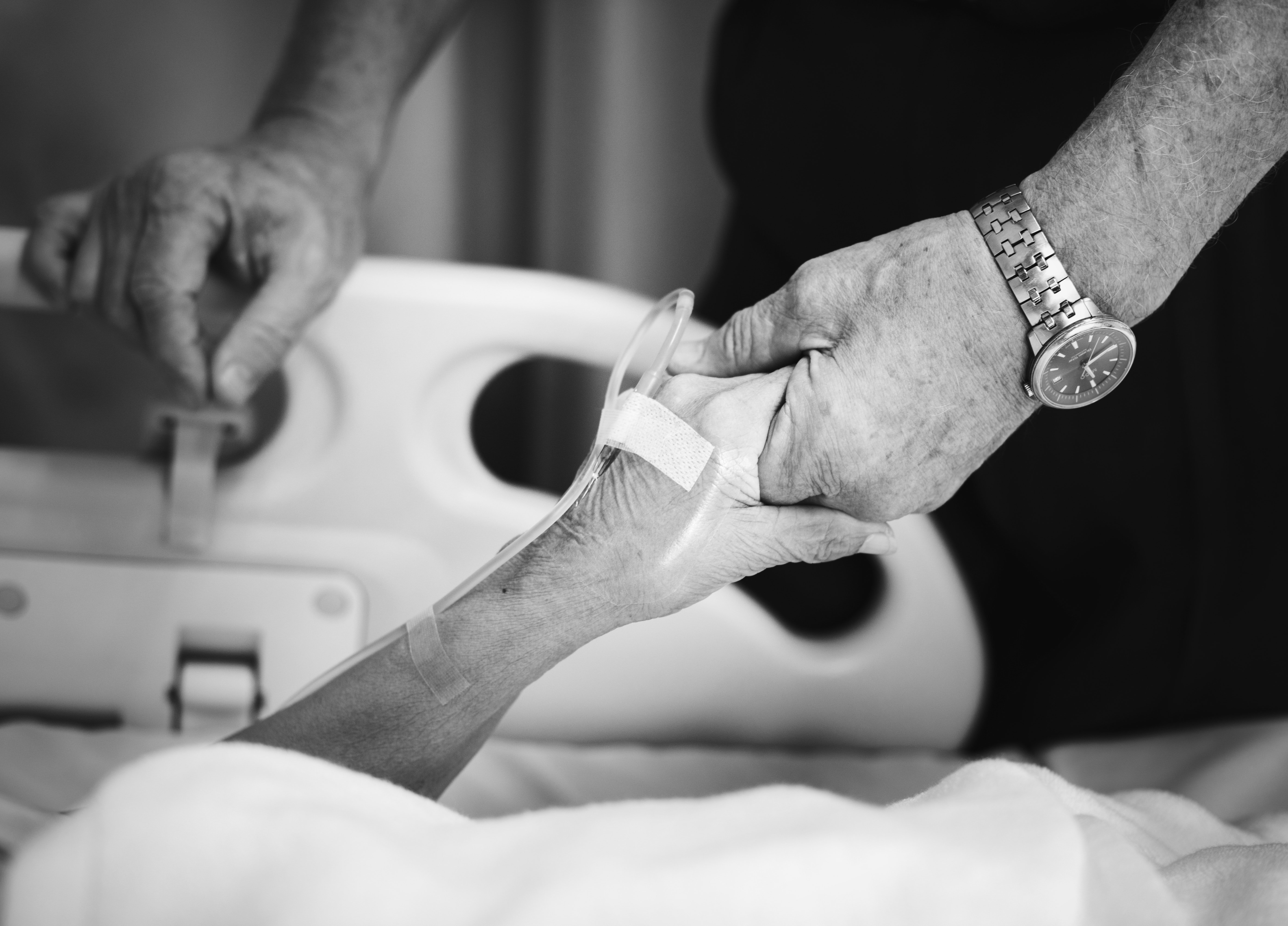
Opening the conversation about palliative care
Palliative care is often misunderstood, with many assumptions of what it’s about. In reality, palliative care helps improve a patient’s quality of life until the very end, regardless of age.
Matthew Kettings works as a social worker in the palliative care unit at Hamilton Health Sciences’ St. Peter’s Hospital (SPH). The unit is one of the largest in Canada and provides a holistic approach to care while managing pain and symptoms.
The scope of social work
The SPH palliative care unit consists of social workers, physiotherapists, occupational therapists, therapeutic recreationists, speech-language pathologists, dietitians and spiritual staff. All provide professional end-of-life care to those with critical illnesses.
“This may seem odd to the audience outside of our unit, but laughter is much more common here than you think.”
Kettings works closely with patients and their families to help them make decisions that preserve comfort, spirituality, autonomy, and dignity for every patient, which may look different for every individual.
Despite the sensitive nature of his work, Kettings notes that laughter is common in the unit.
“This may seem odd to the audience outside of our unit, but laughter is much more common here than you think,” he says. “I’m privileged to spend quality time with patients and their families to learn more about them, and what’s important to them. My job requires understanding patients’ goals and essential information for better care.”
Kettings also offers financial support resources, discharge planning, crisis intervention, supportive counselling and safety planning.
Every situation is new and unique

Fred Cox, a palliative care patient, enjoys a visit with Kettings at St. Peter’s Hospital.
When seriously ill patients discuss their goals of care, considerations include their comfort level, priorities, and preferred care location. Making the best decisions for their care can be challenging.
Kettings assists with coordinating referrals, home care, and outreach services from palliative care teams. “I meet with new patients to help support their transition into the unit while asking questions such as who I can contact to ensure their loved ones know they’re safe,” says Kettings.
“As patients settle into this new stage of life, every situation is new and unique,” says Kettings. “Every patient requiring social work interventions is met with compassion and open-mindedness.”
Patients are encouraged to bring personal belongings from home to make their stay more comfortable, and many also decorate their rooms for holidays with staff’s help. “Several patients, who are very holiday-driven, decorate their space for Christmas and Halloween, giving out candy and presents at times,” says Kettings.
More than a hospital
Within the unit, there are many activities and spaces to help promote overall well-being, including areas for painting, drawing, and cooking.
“We have a wonderful therapeutic recreationalist who can support anything from baking cookies to arranging a space for families to have their meals together,” says Kettings. “Additionally, staff members support activities like bocce, yoga and mindfulness exercises, while also creating spaces for those who wish to be more private.”
During the pandemic, visiting restrictions were in place at SPH. However, the medical team found a way for one patient to have a special visitor.
“There was one patient of mine who had a great-grandchild born during this time but was only able to see them through Zoom calls,” says Kettings. “We arranged a surprise window visit with his granddaughter so he could meet the great-grandchild ‘in person’ through window visiting. We were all quite emotional that afternoon as it was a reunion that had everything stacked against it but we made it work.”
Kettings’ work is not necessarily just within the four walls of a patient’s room. “I’m not always at the bedside with patients,” says Kettings. “The care we provide extends so much more than that.”
Age is no barrier to palliative care
“I think one of the great myths about palliative care is that it’s strictly for the elderly who are dying, and not for those who are younger with complex medical conditions and symptoms,” says Kettings. “I encourage families and patients to advocate for this with medical teams or family physicians. Our population for our unit at St. Peter’s is 18 years of age and up. Age, sex, culture, gender, and race should be barriers we dismantle for palliative care.”
“To provide successful palliative care, it’s not the medical team telling you what is best, it’s you telling your medical team what is important to you, and how we can support you.”
Kettings recently worked with a patient in her early thirties who had very complex care needs. “Despite her illness, she had a resilient and humorous way of interacting with others,” says Kettings. “This patient was exceptional at demonstrating that not everyone in adult hospitals receiving end-of-life care is elderly.”
Palliative care can be included in a patient’s care plan from the beginning of a diagnosis, leading to the end of life. Although it may be a hard topic, initiating palliative care in the earlier stages of a serious disease provides practices that help improve the quality of living.
Kettings adds, “To provide successful palliative care, it’s not the medical team telling you what is best, it’s you telling your medical team what is important to you, and how we can support you. These aspects of life outside of the hospital are important, and should continue within palliative care settings too.”
Inspired by patients and co-workers

Kettings works with families to provide resources and support during the transition to palliative care.
Kettings says he’s inspired every day by his patients, families, and his team.
“I take great pride in working alongside our physicians, allied health team, and exceptional nursing team that consistently goes above and beyond,” says Kettings. “Along with my patients and their families who welcome our staff into their care, this is what inspires me to do my job every day.”