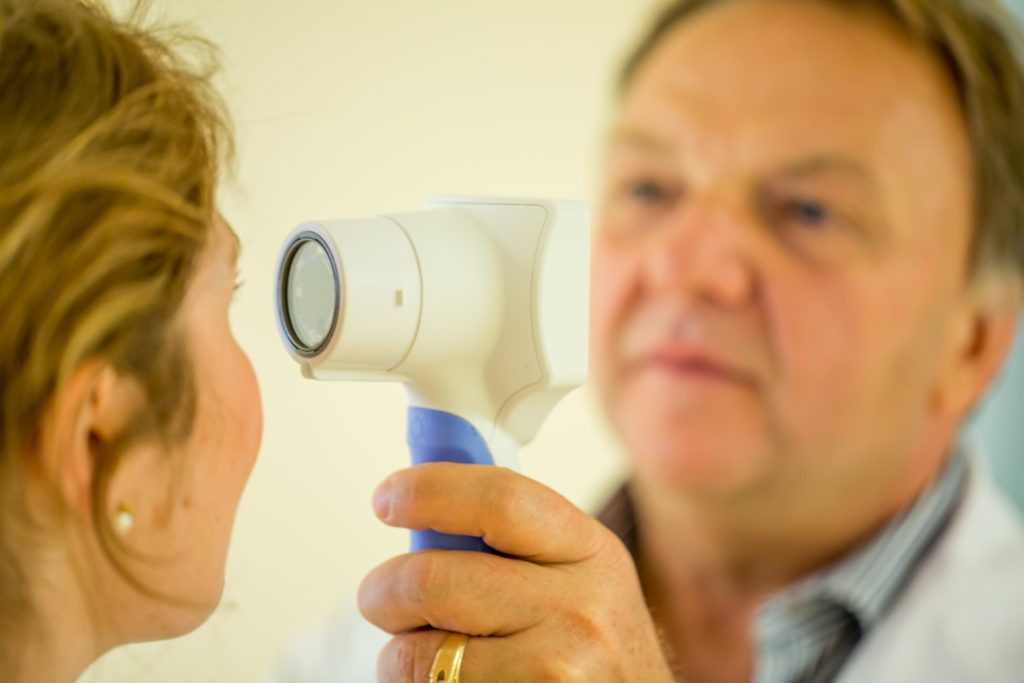
Pupillometer more effective than naked eye
The practice of checking a patient’s pupils to determine how well their brain is functioning has existed for over 100 years. A nurse shines a light into the person’s eye and records how his or her pupils react, labeling them “brisk”, “sluggish” or “non-reactive”. It’s an important exam because it can give the health care team clues about brain activity and indicate whether urgent surgery might be necessary.
“It will give us an opportunity to intervene before it worsens.”
But this method is prone to human error. A variety of factors such as the brightness of the flashlight or varying perceptions of pupil size mean that results can be inconsistent. Small changes in reactivity may not be noticed until the brain is already in danger. To take the guesswork out of this process, Hamilton General Hospital (HGH) has adopted a new technology called a Pupillometer. HGH is one of only five hospitals in Canada using this device.

Dr. Draga Jichici, a neurologist at HGH, says it will improve how quickly they can react to small changes in a patient’s brain activity. “It will allow us to have an objective early warning sign that patients are deteriorating,” he says. “It will give us an opportunity to intervene before it worsens.”
Instead of relying on the human eye to gauge reactivity, you point the Pupillometer at the pupil. Using infrared light, it records a video of the pupil and analyzes it to decide how reactive it is. Instead of using subjective terms like “sluggish” the Pupillometer gives a rating from 0-5. A score of 3 or greater indicates a normal reaction. 1 or 2 indicates that the pupil is less reactive than normal and a score of 0 means it isn’t responsive at all. These scores are stored in the device and can be compared over time to track changes in the patient’s reactivity.
“These changes may indicate that we need to check the patient more frequently, order certain tests or perform emergency surgery on the brain.”
The ability to track changes based on the numeric rating scale will help clinicians to develop the best plan of action for that patient. In some cases, this could mean the difference between life and death.

“The pupil’s changes can precede life threatening changes for the patient,” says Dr. Jichici. “These changes may indicate that we need to check the patient more frequently, order certain tests or perform emergency surgery on the brain.”
The Pupillometer is already in use in the Neurosciences Unit at HGH and is in the process of being introduced to the hospital’s Intensive Care Units.
