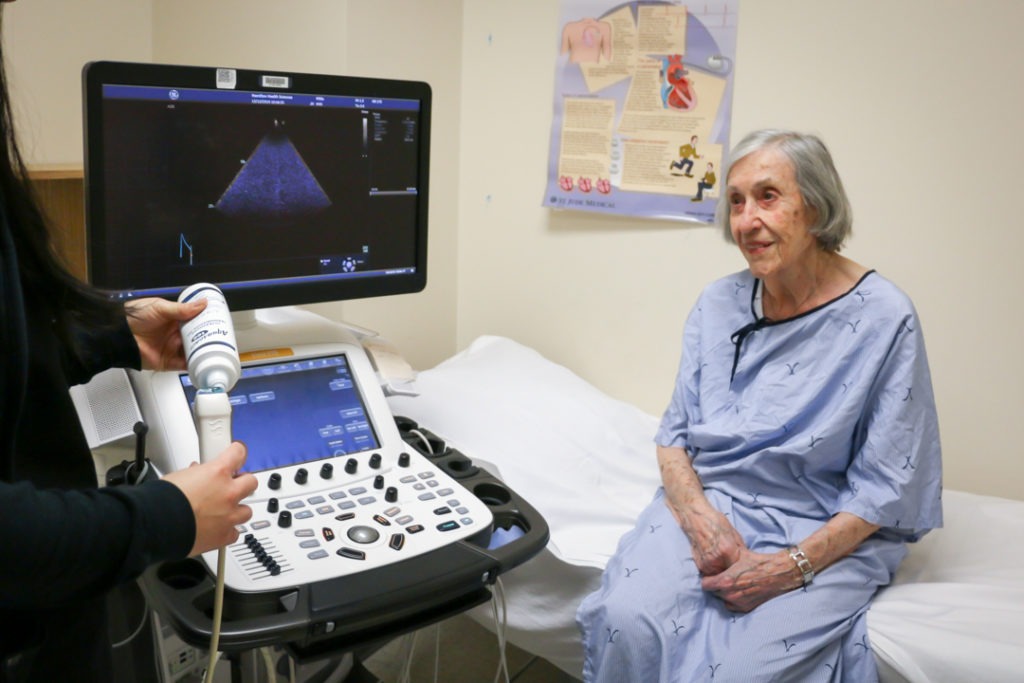
A smoother recovery after heart surgery
Hamilton Health Sciences’ cardiac program is leading the way with new developments in Trans-catheter Aortic Valve Replacement (TAVR), also known as TAVI (Trans-catheter Aortic Valve Insertion). The hospital has been a Canadian pioneer in the minimally invasive procedure over the past decade, and has performed over 900 TAVRs since 2008. This latest advancement focuses not on what happens during the surgery, but after it.
Making minimally invasive heart surgery even more seamless
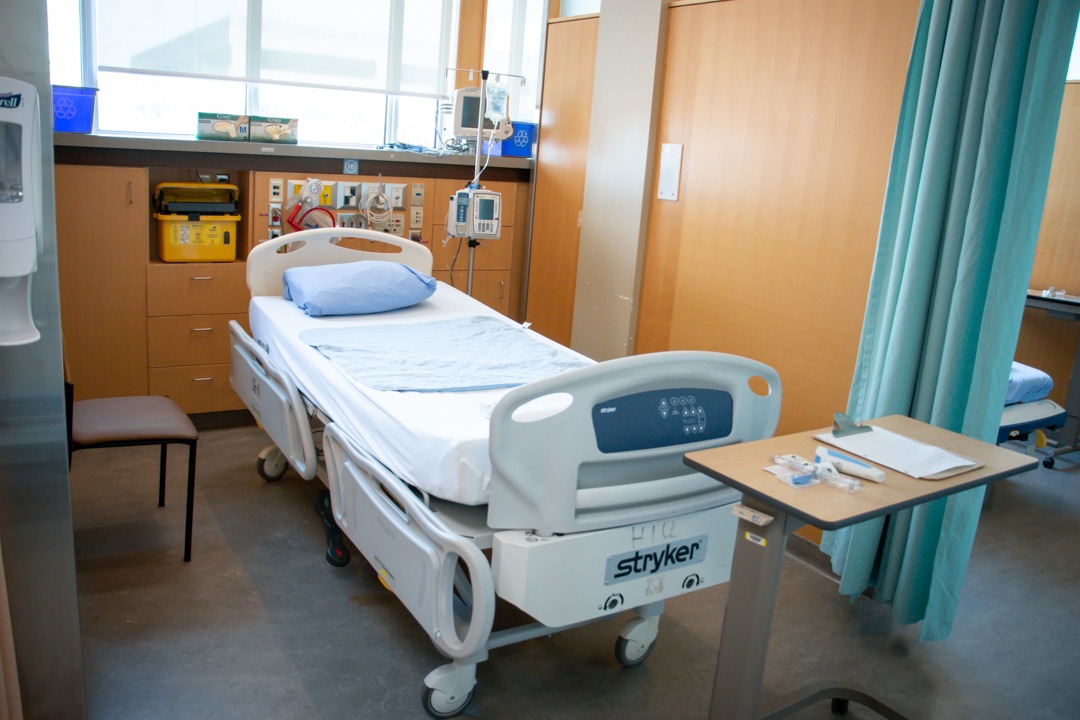
Since November 2019, eligible TAVR patients have been recovering overnight in the Heart Investigation Unit (HIU) where their procedure is performed, rather than being transferred to an Intensive Care Unit (ICU).
“Our goal is to make the entire experience as minimally invasive as possible for the patient and families. We are one of the first in Canada routinely doing this,” says Dr. Madhu Natarajan, a cardiac interventionalist, director of the HIU.
The TAVR procedure, which replaces a damaged heart valve, is done through a small incision in the groin. A catheter is inserted, and the team threads the replacement valve up through the catheter to implant it in the heart.

The red item is a model of a healthy heart valve. The grey item is a model of an unhealthy heart valve. The item in front is the replacement valve that is inserted during TAVR.
When the cardiac team at HHS began performing TAVR, the surgery took roughly four hours, and patients stayed in the hospital for an average of four to five days afterward. With advancements in technology and skill, the procedure now takes under an hour. It’s done under conscious sedation, so the patient is awake. They stay overnight and are generally discharged home the next day.
“We monitor our data very carefully, and saw that 80 per cent of patients were going home the day after their surgery,” says Amanda Smith, the nurse practitioner in the TAVR program. “They were being admitted to the coronary care unit, which provides intensive care for heart patients, and then being discharged the next day.”
Why recover outside the ICU?
The team explored how to operate more efficiently and improve patient safety. They decided that the HIU was the ideal place for an overnight stay for these patients, because:
• Patients aren’t exposed to the intensive care environment where infection is more common. An ICU is also a very expensive place to care for people.
• There is less pressure to access available inpatient beds, which must be prioritized for emergency cases over scheduled surgeries.
• The same team follows a patient from admission to discharge. Dedicated TAVR nurses oversee patient care, and can devote more time to getting patients moving after surgery, which improves outcomes.
“This continuity is very important,” says Dr. Tej Sheth, co-director of the Cardiac CT Imaging Program, who has led the development of the new process. “We are reducing handover between different teams which reduces opportunity for communication errors. This continuity also allows the family to get to know one team, and better support their loved one.”
Remote monitoring makes the process easy for patients
When patients go home, they are equipped with an easy to use monitor that tracks their heart rhythm. They get a follow up phone call from their nurse a few days later to check on their progress. The next month, they return to the hospital to make sure their new valve is functioning well.
Madeleine, 93, was one of the first patients to have a TAVR procedure using this new process. She was impressed with how seamless the experience was.
“When I came home, my granddaughter said to me, ‘can I see the cuts?’” she recalls. “I said to her, you’ll need binoculars!”
She says her overnight stay in the HIU was pleasant, and she was surprised by how easy everything was from start to finish. She lives alone, and does her own cooking and cleaning. She was glad to be able to return to these tasks shortly after her TAVR.

Amanda and Drs. Sheth and Natarajan agree that the new process has been a great success so far. They continue to track measures like readmission to the hospital after surgery to make sure the protocol is accomplishing what it should. They expect to see even more progress in the TAVR procedure in 2020, and are exploring the option of same-day discharge for certain patients.
“We have a wonderful team and everyone is eager to advance the services we offer,” says Dr. Natarajan. “With such great enthusiasm and expertise, we’ve been able to stay on the leading edge of cardiac care.”
