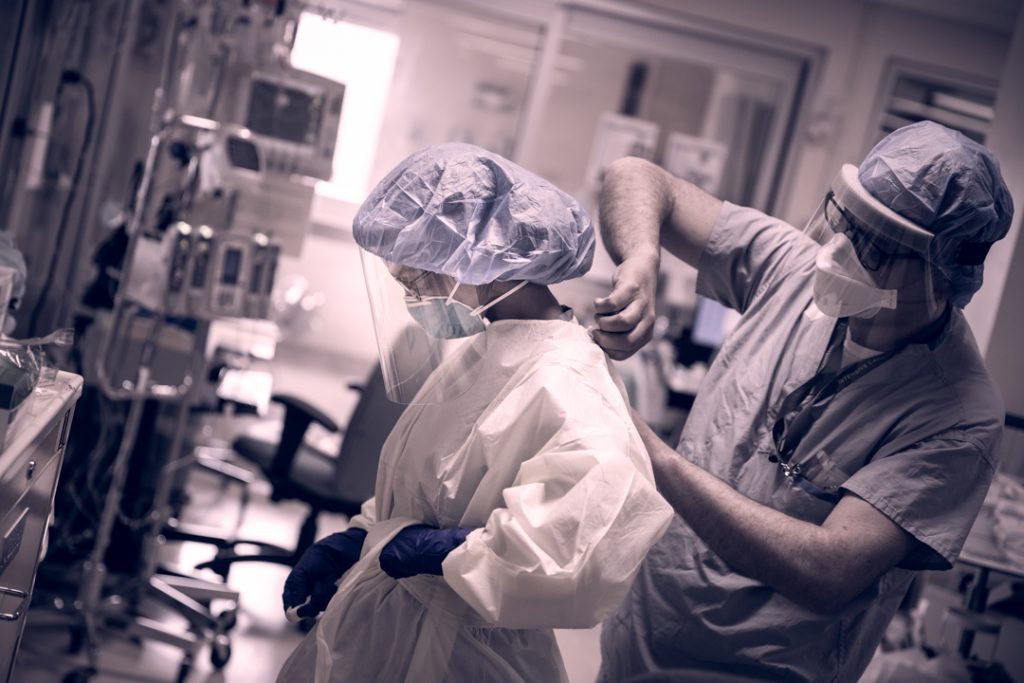
The faces and logistics of the HHS ICUs: Battling the third wave
Hamilton, ON – Teams across Hamilton Health Sciences, like all other hospitals, are under significant pressure as hospitalizations for COVID-19 and variants of concern escalate rapidly. ICU capacity is being severely stretched.
Staff and physicians have worked hard in recent weeks to create more critical care capacity. This has included adding more beds and also redeploying people, updating their skill sets and transitioning to different environments.
By the numbers:
- HHS has increased the number of ICU beds at the Hamilton General and Juravinski Hospitals by 43 per cent, from 88 to 126 overall
- HHS has redeployed almost 200 staff and more are needed
Each ICU bed includes an array of equipment to support patient care. The increase in capacity and equipment has required the doubling up of beds in some rooms and putting ICU beds in areas normally reserved for procedural care.
A team is required to care for one ICU patient. This team includes nurses, physicians, respiratory therapists, infection control and prevention team, social workers, perfusionists, dietitians, pharmacists, occupational therapists, clinical educators, physiotherapists, speech language therapists, health care aides, business clerks and porters.
For staff and physicians, the daily pressures are significant and matched only by the determination to provide the best care for patients:
“We have been doing this for a year, we are more than exhausted. We are no longer the frontline or the last line. The public needs to save themselves. We are seeing multiple family members, within a family die from Covid-19 because they feel their holiday and family gatherings are more important than their lives. We are not coping, we are showing up because we are nurses and that’s what we do.”
̶ Cindi Neptune, ICU Nurse, Level 1 Trauma ICU, Hamilton General Hospital
“As a social worker in the ICU, much of my job has become focused on supporting families of loved ones who are extremely sick or dying from COVID-19. My days are long, busy, and emotionally exhausting. Please think of everyone working in the hospitals and these families when you’re considering whether or not to follow public health guidelines.”
̶ Jodi Konior, Social Worker, Hamilton General Hospital
“Every day is controlled chaos. The ICU is operating over capacity all the time. The nurses, respiratory therapists and doctors are stressed but working hard to care for patients as best as they can, including the staff that have been redeployed from other places. There’s no way we would have gotten through this without each other. We know stay-at-home and other public health measures are hard on everyone, but from our perspective in the ICU, they are absolutely needed.”
– Dr. Bram Rochwerg, ICU Juravinski Hospital Site Lead, Associate Professor of Medicine, McMaster University
All media is invited to share the quotes and insights of our ICU team, and their images, available through the below link to inform and educate the public about why it is up to everyone to do their part to get through this crisis – https://www.hamiltonhealthsciences.ca/wp-content/uploads/2021/04/A-day-in-the-life-in-an-ICU-experiences_April-27.pdf
More information, including ICU capacity data, has been added to our website at https://www.hamiltonhealthsciences.ca/covid19/.
– 30 –
Previous Media Updates:
- HHS ramping down some scheduled and non-emergent care – April 9
- HHS taking additional measures to create critical care and staffing capacity in response to the third wave – April 16
- Update: HHS’s ongoing effort to create critical care and staffing capacity – April 21
For more information, please contact:
Wendy Stewart
Communications & Public Affairs
Hamilton Health Sciences
stewartwen@hhsc.ca
