Getting self-assured: Hospital Elder Life Program adjusts to provide care during COVID
Malise Lynch was recently admitted to the Hamilton Health Sciences’ (HHS) Regional Rehabilitation Centre following surgery at Hamilton Health Sciences’ Juravinski Hospital and Cancer Centre. She fractured her pelvis in a fall two weeks ago at the Dundas retirement home where she lives.
“I know the centre will help me learn how to walk and be totally independent again,” says Lynch. “You have to be totally independent to live at my retirement home. I’ve always been that way – I even say my middle name is ‘Independent.’”
HELP me if you can, I’m feeling down
Lynch is one of the many patients at HHS who benefit from HELP – the Hospital Elder Life Program. The program’s mission is to prevent delirium, a sudden and usually temporary state of confusion. Some studies show that prevention strategies used by the HELP program can reduce the delirium rate in hospitalized elders by up to 40%.

Kelly Turner, elder life specialist at Hamilton Health Sciences.
HELP works with patients across several units at the Juravinski Hospital and Hamilton General Hospital. The team itself consists of elder life specialists, elder life clinical nurse specialists, a geriatrician, and volunteers. Volunteers account for approximately 50 to 100 people on the team, depending on the time of year due to university students and co-op placements.
As a result of the pandemic, in-person volunteering has been put hold – meaning staff have had to find other ways to keep HELP patients physically and mentally active.
“Our staff team is quite small, only five people,” says Kelly Turner, elder life specialist at HHS. “We have very well-trained volunteers who would normally help patients at their bedside, if not for the pandemic. They’d deliver targeted HELP interventions such as orientation, therapeutic activities, meal assistance, mobility assistance, and sleep promotion.”
And I do appreciate you being ’round
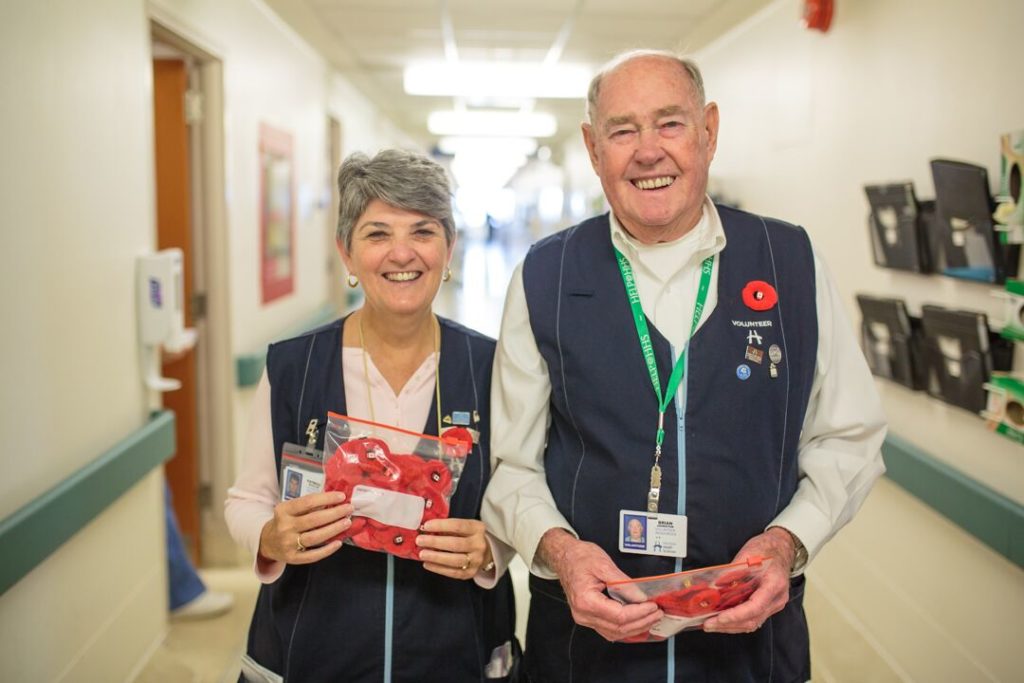
With COVID pressing pause on in-person volunteering, some of the elder life specialists decided to make senior-friendly activity kits with a range of delirium prevention resources they could provide for patients. Kits include a range of activities to promote cognitive stimulation such as puzzles and colouring pencils; ear plugs and eye masks to encourage proper sleep; stress balls for exercising hands; and delirium education materials. “The kits have been very well-received by both unit staff and the patients.” Turner says.
HELP me get my feet back on the ground
While the kits have been a welcome support for patients, human interaction is still an important aspect of the program and as a result, HELP developed a phone program to fulfill this need.
“We set up an internal website that volunteers are able to access securely from home,” Turner explains. “On the website, volunteers can access a care plan designed for each patient and call the patient every day to carry out delirium prevention interventions over the phone.”
“She cannot put into words how grateful she is to have these phone calls”
Patients like Lynch are happy to receive those calls. Alessia Macaluso is one of the HELP volunteers working with Lynch. “She’s told me that she is so moved that this program exists and that people would volunteer their time to call seniors who are alone in the hospital,” Macaluso explains. “She said it makes her feel connected and she cannot put into words how grateful she is to have these phone calls.”
March 17 is World Delirium Awareness Day. You can learn more about HELP here.