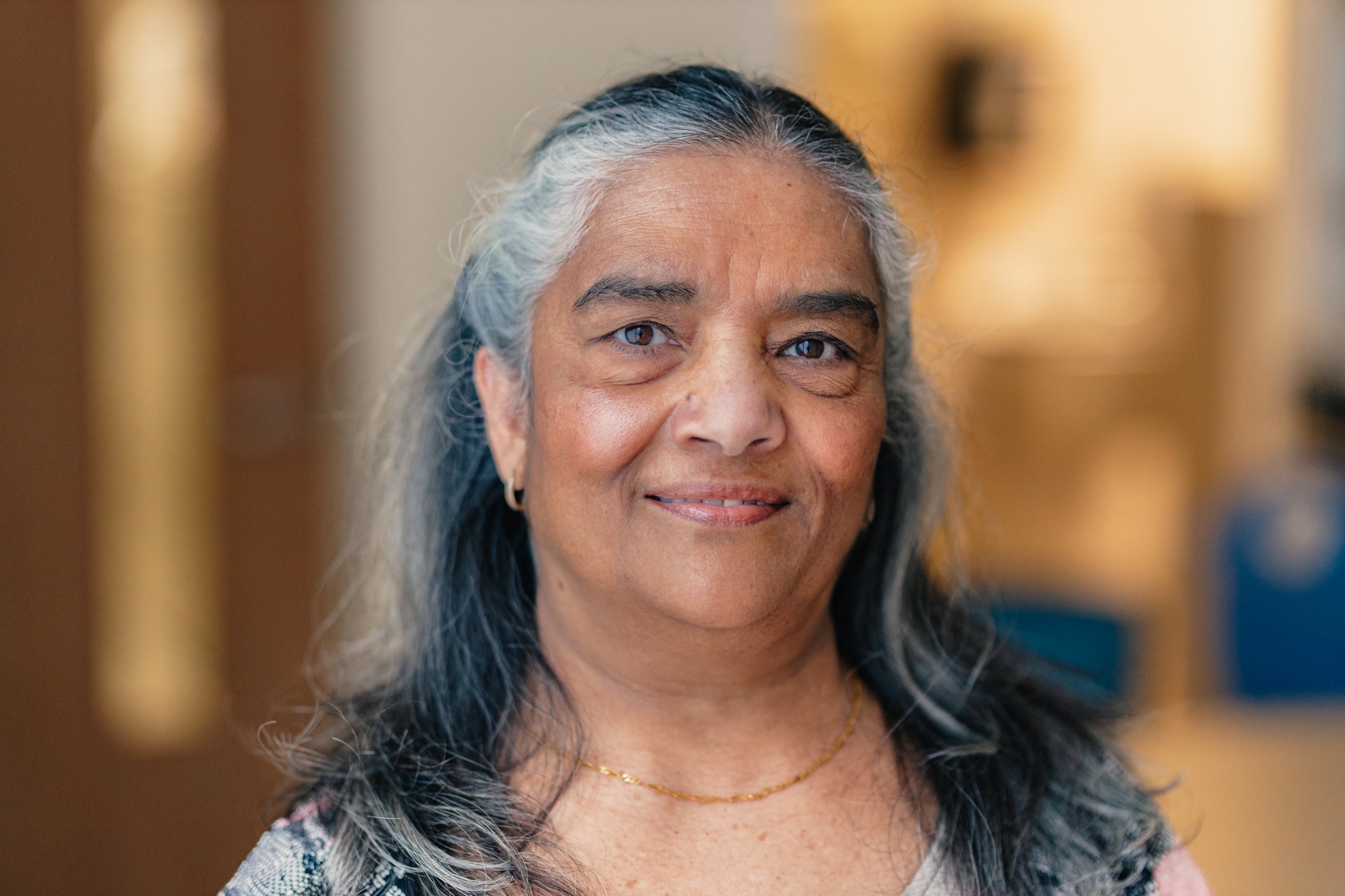Introducing a Medical Radiation Technologist in Interventional Radiology
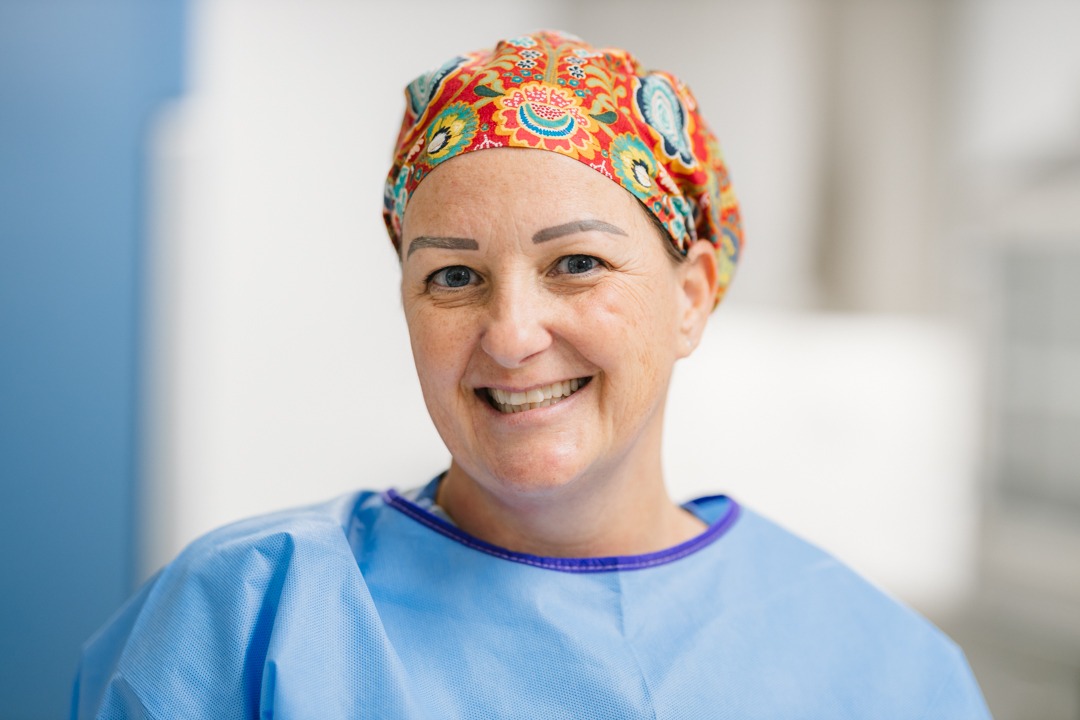
Kayleigh Kulla began her career with Hamilton Health Sciences (HHS) six years ago, after a successful student placement in her final year of university. She has worked in three different areas of Diagnostic Imaging – located at HHS’s Juravinski Hospital and Cancer Centre: general X-ray, computed tomography (CT), and interventional radiology.
Last month, HHS began to introduce staff who work in the Medical Radiation Technologist profession. For this week’s Introducing profile, we spoke to Kulla about interventional radiology – what it is, treating patients, and some of the challenges and rewards that come with being in her line of work.
Tell us – what is interventional radiology?
Interventional radiology is a part of diagnostic imaging that specializes in minimally invasive procedures. The interventional radiology department is similar to an operating room, except most of our procedures are done under conscious sedation rather than general anesthesia.
We perform biopsies, embolizations, and drain insertions. Doctors use the results from these tests to diagnose and treat patients.
Most people have likely heard of a biopsy, but perhaps not embolizations. It’s a type of therapeutic treatment used to block blood flow to a certain area of the body – this can shrink tumours to stop internal bleeding. One of the more common types of embolization procedures we do is called TACE, which stands for transarterial chemoembolization (TACE). In short, it’s a way to treat liver cancer. Being a cancer hospital, we do a lot of TACEs because it is a procedure to treat liver cancer by blocking blood supply to liver tumours and administering chemotherapy directly to the tumour. Most of our common embolizations involved cutting the blood supply off to a tumour or mass.
 What are some of the day-to-day responsibilities of someone in your line of work?
What are some of the day-to-day responsibilities of someone in your line of work?
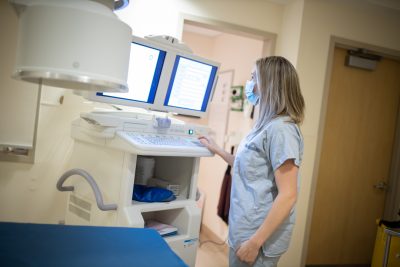
As an interventional technologist, my job is to prepare patients for procedures, assist them onto the procedure table and position them accordingly, and set them up on the vitals monitor. I also operate the imaging equipment required for the patient’s procedure and perform post-processing of imaging. Some of the procedures we do require special imaging called angiography, which uses “real-time” X-rays to visualize blood vessels. All interventions are done using a sterile technique so we also help set up sterile trays. I sometimes screen patients, such as review their bloodwork, but usually one of our nurses will do that.
What are some of the challenges that come with the job? What do you find most rewarding?
Not every case goes as planned, so at times we have to stop procedures. Our goal is to provide the very best care to our patients, so when things don’t go as planned it is frustrating to us, as well as the patient.
The best reward is having patients express how grateful they are for everything we do and knowing how much of a positive difference we’ve made in their lives. They’re fighting extremely hard battles and to be able to help them through the process and up to recovery is an amazing feeling.
Some patients are very anxious when they come to get procedures done, so I will hold their hand if they need it and explain everything step-by-step to help them calm down.
I had a patient who was palliative that came to us numerous times for a variety of procedures. After one of her procedures, she said, “you know, I have terminal cancer. I’m dying and it really sucks. But you made it suck a little bit less.”