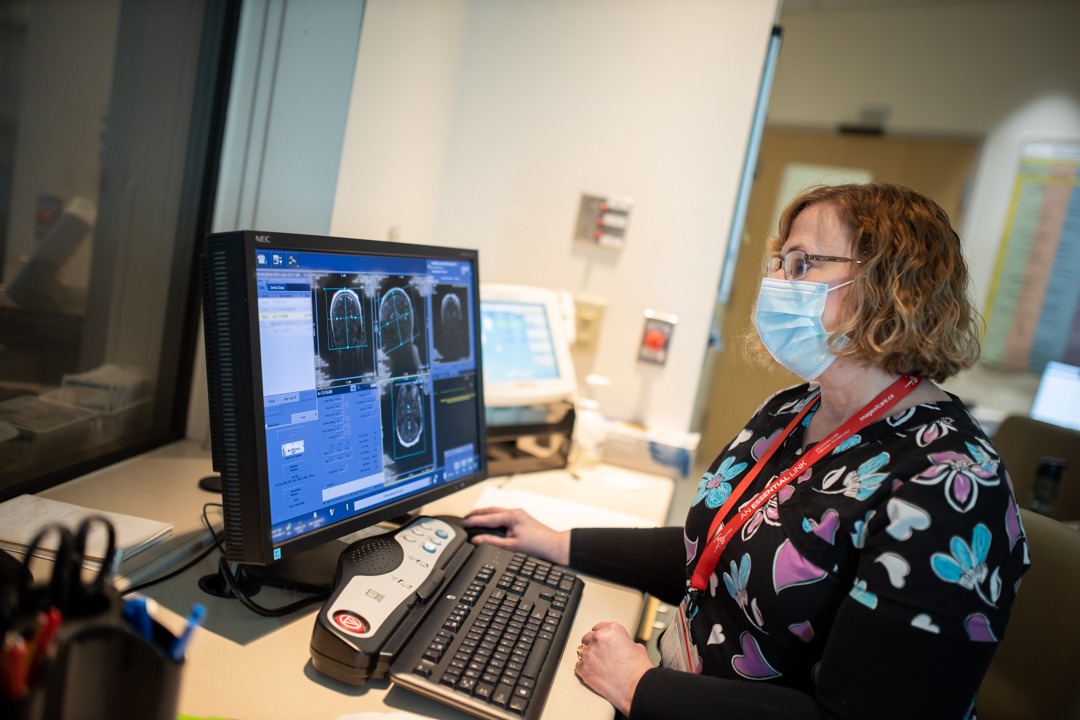
Introducing a Mammography Technologist
This profile is part of our Introducing MR Tech series to highlight the work of our diagnostic imaging unit.
Working in mammography wasn’t always on Lauren Harris’s radar when it came to growing into her career in diagnostic imaging (DI).
“When you’re studying to become an X-ray technologist, mammography is not touched on as much as the other areas of diagnostic imaging,” Harris explains. “When I worked at a clinic in Burlington as an X-ray tech, they asked if I had any interest in mammography and I took the opportunity. I had on-the-job-training and I really liked it.”
Harris’s career at Hamilton Health Sciences (HHS) started in 2012 on a casual basis in the DI unit at the Juravinski Hospital and Cancer Centre. In 2016, a part-time opportunity opened up at the CIBC Breast Assessment Centre at Juravinski Hospital and Cancer Centre. She’s been there ever since.
What’s the biggest difference between working in X-ray and working in mammography?
I would say the biggest difference is the need for really good communication skills. You’re up close with patients in mammography. Our patients are more nervous about their exams, so you need to learn how to ease their anxiety. It’s different if you’re getting an X-ray done for a broken finger, rather than a mammogram for cancer screening. You have to be quick to develop relationships with patients to help ease their fears.
What are some of your daily responsibilities?
The bulk of our work is cancer screening. The majority of our patients are in the Ontario Breast Screening Program (OBSP); it’s a self-referral program for women in the 50 to 74 age range. Most of the patients we see do not have symptoms of breast cancer and are considered asymptomatic, so they’re coming every year or every two years based on radiologist recommendations. Another portion of our work is performing surveillance mammograms. These are for patients who have had breast cancer before and are coming back for yearly check-ups. The remaining patients are people who have concerning breast symptoms. Their mammograms may lead to further imaging like an ultrasound or biopsy.
As a technologist, I assist the radiologists in different procedures such as breast biopsies. We spend a lot of time with the patients during these procedures, too, explaining what’s going to happen, obtaining their consent, and getting them ready.
We also work really closely with the radiologists. We review specific mammogram cases with them and then relay the results and information to patients based on what the radiologist has determined.
Another group we work closely with are ultrasound technologists. We do the first step of a patient’s imaging – the mammogram – and if an ultrasound is required, we relay information to the ultrasound tech based on the radiologist’s requests.
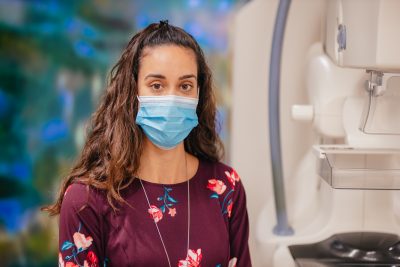
Harris says, “We advise women that the benefits of screening mammography outweigh the possible risks.”
What are some of the challenges that come with your position?
The main one is definitely helping a patient through their anxiety and nervousness. Patients react to being fearful in different ways; sometimes it’s anxiousness, sometimes it’s anger. Other times they’re very emotional. I have to tell myself that they’re not angry at me, it’s just how they’re expressing their fear.
Another challenge is patient education. Some people don’t believe in mammograms because of misinformation they’ve read. We advise women that the benefits of screening mammography outweigh the possible risks. The amount of radiation exposure from a mammogram is about the same as a one-way airplane flight from southern Ontario to Vancouver. Getting screened regularly with mammography is important because it can find cancer early when it is less likely to have spread to other parts of the body. Treatment may also have a better chance of working when breast cancer is found early.
There’s also misinformation out there about the Ontario Breast Screening program. It’s a self-referral program for women who are 50-74 years old, so some may feel that once they’re out of that age range they shouldn’t go for regular mammograms. Women over the age of 74 can be screened within the OBSP; however, they are encouraged to make a personal decision about breast screening in consultation with their healthcare provider.
What’s your advice for someone who’s interested in working in DI?
I would say you have to have good communication skills to work in any part of DI. I learned this especially when I moved to mammography. The art of good communication is the biggest asset to the job – being able to answer people’s questions and try to lower their anxiety as they go into their appointment is huge.
Another skill you need is problem-solving. Not every patient you see is going to be able-bodied. Sometimes we have patients with mobility issues. We have to be creative and adapt the procedure to the patient.
Are there any positive patient experiences that stick out to you?
Before the pandemic, we had volunteers who’d hand out surveys to our patients asking about their experience with us. At our weekly team meetings, our manager would read out some of them, saying that we made their experiences better. That was always a nice way to start our day. Our booking clerks will sometimes get patients who ask specifically for you to do their mammogram, saying they had a really good appointment last time and would like to have you again. Or sometimes you meet someone in the waiting room and they say they remember you from their last visit. Some patients will mail a thank you card to the entire team to show their gratitude.
Today is World Cancer Day, an international day marked on Feb. 4 to raise awareness of cancer and to encourage its prevention, detection, and treatment.