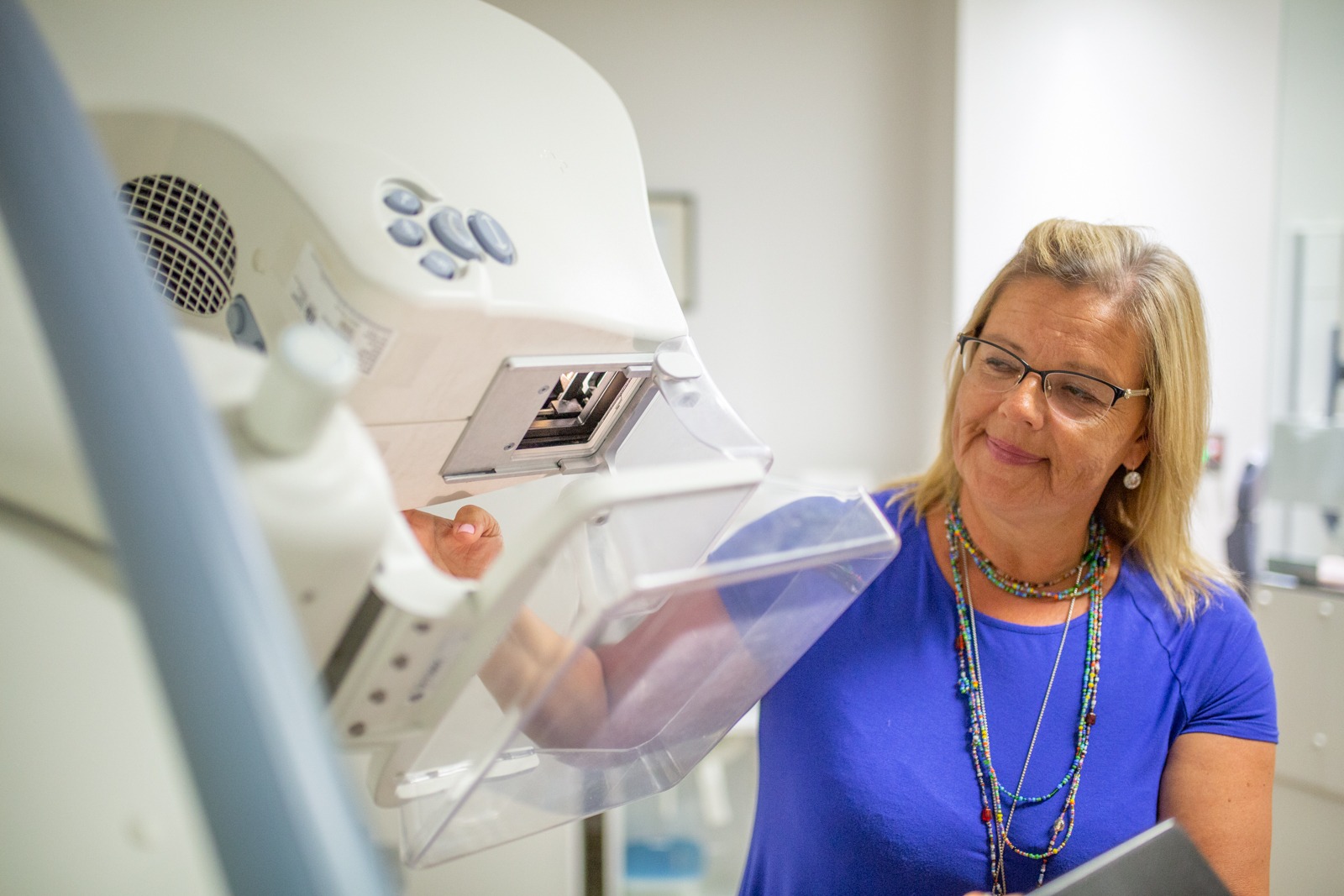
Health Tip: What to expect from a mammogram call-back
After you’ve gone for a mammogram to screen for breast cancer, most of the time those x-rays are clear. But what happens if you get a call back after your test? Here’s what to expect during your follow-up visit at Hamilton Health Sciences (HHS)’ Breast Assessment Centre located at Juravinski Hospital and Cancer Centre.
About 10 per cent of people who get mammograms will be called for a follow-up appointment that will include more mammography and possibly also a breast ultrasound, MRI and/or biopsy. In most cases, these additional tests rule out breast cancer. But they’re important to do because the earlier breast cancer is diagnosed and treated, the better the outcome.
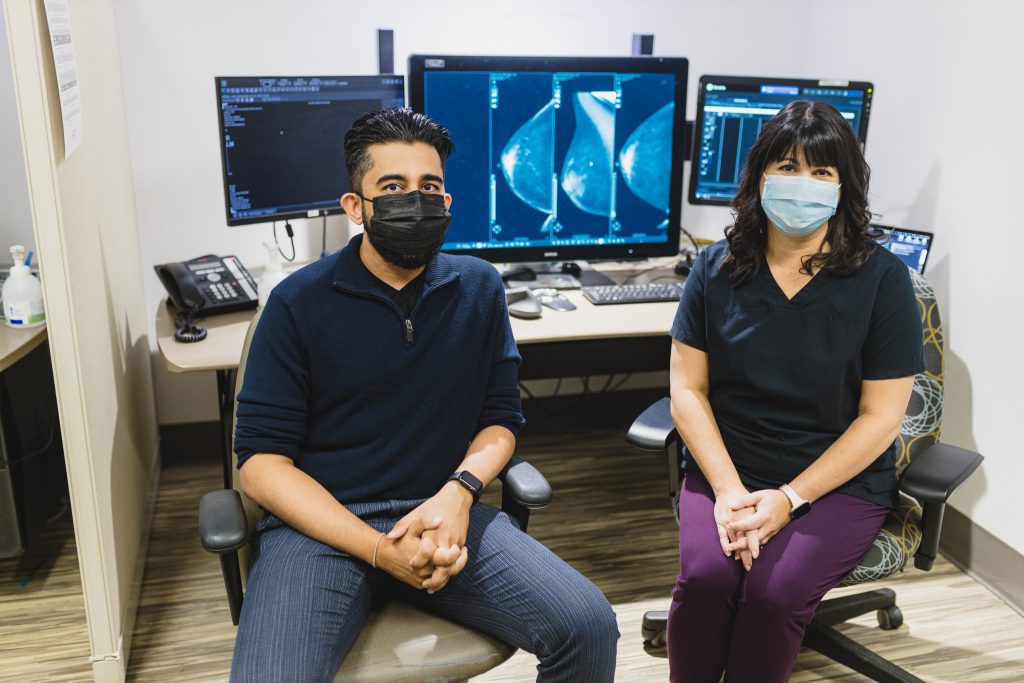
The Breast Assessment Centre at HHS is among the most advanced breast screening and assessment centres of its kind in Canada. Patients receive results quickly – often on the same day as their appointment – because of a coordinated approach that brings together radiologists, surgeons, pathologists and other breast care experts in one location.
Follow-up tests typically start with additional mammograms.
More mammograms
These extra breast x-rays are done for a closer look at the area of concern, says mammogram technologist Rita Iamarino. In most cases, patients are recalled for benign (non-harmful) findings or to confirm normal breast changes.
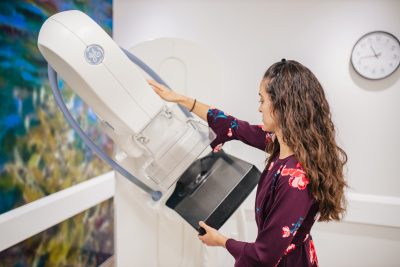
A mammogram technologist with a mammography machine
Preparing for these extra x-rays and other follow-up tests is much the same as preparing for a mammogram. A radiologist examines the additional images to determine whether more tests are needed while the patient waits, says Dr. Prasaanthan Gopee-Ramanan, an HHS diagnostic radiologist specializing in breast imaging. If no further tests are needed, the patient goes home.
If more tests are needed to either rule out or diagnose breast cancer, the patient stays for additional tests that could include more breast x-rays including a 3D mammogram, a breast ultrasound, breast MRI and/or a biopsy. The MRI and biopsy could also be booked on another date, as soon as possible.
Breast ultrasound
A breast ultrasound shows images using sound waves. It helps the radiologist learn more about the irregularity in breast tissue, and can show whether it’s a fluid-filled cyst or a solid mass, says Gopee-Ramanan. A registered ultrasound technologist performs the ultrasound and shows images to a breast radiologist, who decides the next steps.

Dr. Prasaanthan Gopee-Ramanan is an HHS diagnostic radiologist specializing in breast imaging.
For this procedure, the patient lies face up and/or to one side. Ultrasound gel is put on the skin and may feel cold. The technologist moves a smooth tool, called an ultrasound probe, across the breast. This probe sends sound waves through the breast tissue, creating pictures on a computer screen. The procedure takes about 20 minutes. If the ultrasound shows no need for concern, the patient goes home. Or the radiologist may ask for more tests.
Breast MRI
Magnetic resonance imaging, or MRI, uses magnets and radio waves to produce detailed three-dimensional images of the breast tissue, says MRI technologist Kristine Fisher.
“We have to do a very thorough screening of patients before this test.” — Kristine Fisher, MRI technologist
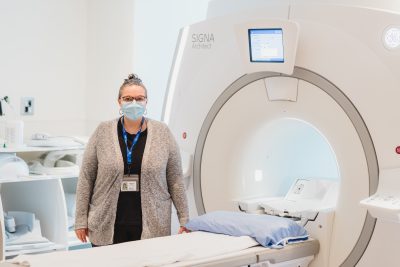
Technologist Kristine Fisher with an MRI machine
Two groups of patients are referred for breast MRIs. The first had something suspicious on other tests, and an MRI was ordered for an even closer look. “The MRI gives more information because it shows all the soft tissues, ducts and vessels in a full 3D mode,” says Fisher.
The second group is considered high risk, and gets an MRI as part of their yearly screening. A patient carrying the BRCA breast cancer gene would fall into this category.
For this test, an intravenous (IV) line is inserted into the patient’s arm so that a contrast dye can be injected during the test. This contrast helps to show any potentially cancerous breast tissue. The patient lies on their stomach on a padded platform with cushioned openings (holders) for the breasts. Each opening is surrounded by a breast coil, which is a signal receiver that works with the MRI unit to create images. The platform slides into the center of the tube-shaped MRI machine. The patient won’t feel anything, but will hear a loud thumping sound from the machine.
“We have to do a very thorough screening of patients before this test,” says Fisher. That’s because the MRI machine uses strong magnets so it’s important that anything metal — such as jewelry and clothing with snaps, belts, and zippers – be removed before the test. The technologist will also ask about any implants, such as a pacemaker or aneurysm clips, and clear any implants for scanning.
The patient needs to stay very still during this test, which takes about 15 minutes. It can take between one and five days for results, depending on the urgency.
Biopsy
The radiologist may also order a biopsy. This could happen the same day as other tests, or be booked on a different day, as soon as possible.
During a biopsy, a small sample of suspicious tissue is removed by a needle so it can be examined under a microscope. The area is numbed first, so the patient won’t feel the procedure. If a biopsy finds normal tissue, the patient returns to routine screening through the Ontario Breast Screening Program.
If a biopsy leads to a diagnosis of non-cancerous breast disease that might require surgery, the patient will be referred to a surgeon to discuss options. If it confirms a cancer diagnosis, the recommendation in most cases is to meet with a surgeon. It takes about two weeks to receive biopsy results. Patients get biopsy results from their family doctor.
Test results
Test results can also be accessed directly through MyChart, a free, secure, online tool that gives HHS patients easy access to their hospital health record.
Patients can choose whether to view results on MyChart, or wait and find out from their doctor. MyChart registration is easy and takes only a few minutes.
October is Breast Cancer Awareness Month. This story is the first in a two-part series on what to expect from a mammogram follow-up appointment, should you receive a callback. Story two, to be published on Oct. 19, shares tips for managing the stress of a callback.