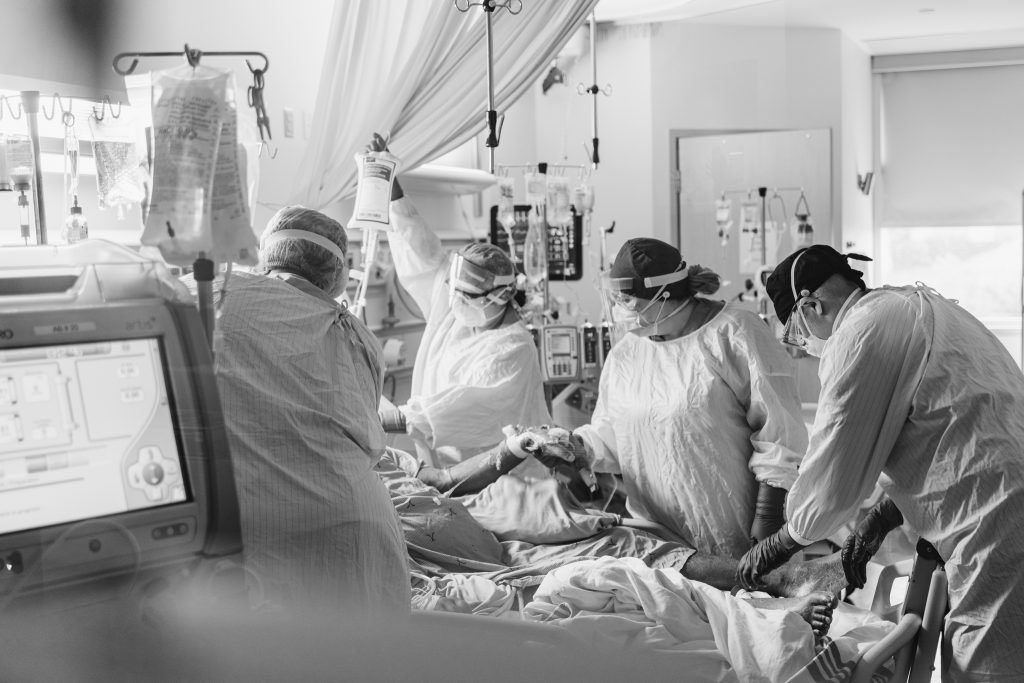
Refusing vaccination can lead to “death’s door” in the intensive care unit
The dire situation in Ontario’s intensive care units (ICUs) is all so preventable, say Hamilton Health Sciences’ (HHS) doctors.
They’re caring for the sickest COVID patients and know all about what it’s taking to keep unvaccinated people alive in the ICU.

Dr. Paul Engels
“It’s sad to see people who could have easily avoided these life-threatening COVID infections with a simple vaccination, now on death’s door,” says Dr. Paul Engels. “Sadly, some will certainly die and leave their families without fathers, brothers, mothers, sisters.”
Engels is an intensivist, which means he is specially trained to care for critically ill patients. He is also a trauma surgeon and a member of the extra-corporeal life-support (ECLS) team, a team that provides artificial heart and/or lung support to those who need it.
“Providing ECMO care to patients with such a high burden of illness can be emotionally and physically exhausting.”
Last resort treatment for critically ill COVID-19 patients
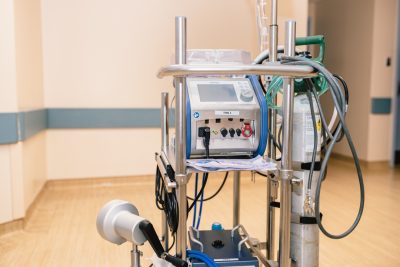
An ECMO machine is a type of life support that acts as a person’s lungs when their own can’t function.
An ECMO (extra-corporeal membrane oxygenation) machine is one way to provide this support.
This cutting-edge type of life support replaces the function of a patient’s own lungs by pumping blood from the patient’s body to an artificial lung (oxygenator) that adds oxygen to it and removes carbon dioxide.
HHS, which is one of only four large hospitals in Ontario to provide ECMO care, introduced the life-saving machine early in 2020.
“These patients are very ill, and their care demands attention to detail and vigilance, and certainly can be challenging to manage,” says Engels.
ECMO is used for a variety of conditions that can cause severe damage to the lungs and/or heart, including pneumonia, trauma, massive heart attacks, and more – but throughout the pandemic, these machines have mostly been used to treat severely ill COVID patients.
ECMO patients require more healthcare resources

Dr. Julian Owen
“The road to recovery is unfortunately long and winding for patients requiring ECMO,” says HHS intensivist and ECLS team member Dr. Julian Owen. “It is tremendously rewarding to see ECMO patients recover to the point of coming off the ventilator, leaving the ICU, and even walking out of the hospital.”
But not every outcome is a favourable one.
ECMO has been used to treat over 8000 patients worldwide, with almost half of them dying in hospital.
Since ECMO patients are the sickest patients, they require constant attention by a large healthcare team.
“It can be very demanding,” says Owen. “Patients are extremely sick and often require other forms of life support in addition to ECMO. There is a high degree of complexity in their care and high stakes for every decision that the team makes.”

Dr. John Centofanti
ECMO patients are at highest risk of complications from being critically ill, including infections, blood clots, bleeding, kidney failure, heart dysfunction and chronic lung disease, says HHS intensivist, member of the ECLS team, and anesthesiologist, Dr. John Centofanti. Older people generally can’t tolerate the physical stress of this type of machine, so it is most often used with younger, otherwise healthier patients.
Care for ECLS patients requires input from physicians, respiratory therapists, nurses, perfusionists, physiotherapists, dietitians, and other specialists such as hematologists, thrombosis physicians, infectious disease physicians, and more.
“Like many of our regional programs, I think HHS has built an incredible team that I am proud to be a part of,” says Owen.
All three doctors say they feel honoured to be able to provide this level of care. But it also has its downfalls.
Centofanti calls it a “tremendous undertaking.”
“Despite these sentiments and dedication, it is also overwhelming to see the level of disease burden COVID brings to previously healthy, young individuals, many of whom are younger or otherwise healthier than me,” he says. “Care for ECLS patients, and on the COVID unit in general, requires more than just looking after the sickest of the sick. It requires attention and focus on caring and looking after the entire team, the level of burnout, and the input they can provide in helping these patients.”
HHS has critical care units at Hamilton General Hospital (HGH) and Juravinski Hospital, but HGH is the only site with ECMO machines.
Pandemic causing healthcare worker burnout
Centofanti fears we have entered a stage where people are “done with COVID” – but healthcare workers know this stage by another name: the fourth wave.
“Lives have been altered, and in some cases, turned completely upside down. I understand the need to return to normalcy and a sense of complacency with new rules, restrictions and guidelines,” he says. “Nonetheless, COVID is not done with us. Viruses have a unique way of trying to survive and prosper, changing, adjusting, mutating.”
Being fully vaccinated against COVID-19 is the best prevention against serious illness, hospitalization and death.
All of the patients with COVID-19 that have required ECMO at HHS have been unvaccinated. During CTV News’ visit to Hamilton General Hospital on September 15, 2021, all of the COVID-19 patients in the ICU were unvaccinated, and eight were on ECMO.
VIDEO: “There’s a catheter the size of a garden hose in his neck, and there’s a catheter the size of a garden hose at his groin.”
“Although 20 per cent of the eligible population of Ontario are unvaccinated, they represent 80 percent of hospitalizations and nearly 90 per cent of ICU patients,” says Dr. Sunjay Sharma, Medical Director at the HGH ICU. “It is very clear that being fully vaccinated significantly decreases your risk of getting seriously sick and hospitalized from COVID-19 – as well as decreases the chance of our hospitals being overwhelmed.”
It’s hard for people to understand what hospital workers are really going through. Take one look at Twitter which acts as a community space for many to see just how they are feeling.
Healthcare workers are frustrated and burnt out.
‘I have seen a tremendous amount of tragedy’: Hamilton doctors speak about the toll of COVID’s fourth wave
👉https://t.co/FZWR8Y3MPr @jfrketich reporting #HamOnt
— Hamilton Spectator (@TheSpec) October 1, 2021
Trigger warning: COVID death.
Hi Jane. This is Dr. Bakshi calling from Edmonton. I am not sure if you’re aware, but your mom Anne was admitted to the COVID ward about 2 hours ago. I’m calling because she is not doing well, and will likely not survive the day.”
— Neeja Bakshi (@NeejaB) September 30, 2021
Going to take a Twitter break for the next 6 weeks, to conserve energy for myself and the people I love! Most of my life happens OFF SoMe, and that’s where I’d like to focus my attention right now. Here’s some parting thoughts: 🧵https://t.co/5h1eMvM281
— Menaka Pai, MSc MD FRCPC (@MPaiMD) August 22, 2021
Just got off the phone with one of my closest friends, who is an ICU nurse at one of the biggest hospitals in the Bay Area. I’m going to share a few quotes from that conversation because I think it’s hard for people to understand exactly what hospital workers are going through rn
— Katie MacBride (@msmacb) August 22, 2021
A new CMA survey explored the impact of the ongoing pandemic on the health of physicians.
🔹Results show high levels of fatigue + anxiety and very few physicians – only 16% – are seeking help. https://t.co/5MFxzjJlEA #CDNHealth #PhysicianHealth pic.twitter.com/AzxQ2pF4Vz
— Canadian Medical Association (@CMA_Docs) March 10, 2021
Once surgeries get cancelled the health system isn’t at risk of being overrun, it is overrun.#COVID19 #medtwitter
— Dr. Alika Lafontaine (@AlikaMD) September 13, 2021
“COVID-19 doesn’t change its virulence or transmissibility as it crosses provincial borders. There are signs this pandemic has overrun, or will soon overrun, health systems. We need all hands on deck to acknowledge that the ship is sinking.” – @AlikaMDhttps://t.co/2KRpa0efYz
— Canadian Medical Association (@CMA_Docs) September 17, 2021
Dear Albertans
I’m BEGGING you to get vaccinated & stay home 🙏
If you get infected today, you (or your loved ones) could land in ICU in 2-3 weeks, & at that point there is a real chance we won’t be able to offer you the care you’ll need.
Signed,
An exasperated doctor
— Ilan Schwartz MD PhD (@GermHunterMD) September 17, 2021
“Providing ECMO care to patients with such a high burden of illness can be emotionally and physically exhausting,” says Owen. “Patients requiring ECMO support are often young and it is difficult to see them fighting for their lives and their loved ones devastated by their illness.”
“I think we are all experiencing fatigue in different ways,” says Centofanti. “A healthy mindset and balance are important for everyone. A cohesive, trusting, and enjoyable group of family and friends help to lighten the load and remind us of the world outside of the ICU, and outside of COVID terror. Prioritizing this is important for ensuring our team is rejuvenated when it comes to providing patient care.”
Please receive the vaccine as soon as you are eligible: https://www.hamilton.ca/coronavirus/covid-19-vaccination.






