
Introducing a Nurse Clinician specializing in skin, wounds and ostomies
Ask Stephanie Furtado to open her supplies cupboard and you’ll find everything from gauze fabric squares to scissors, foam shapes, paste, tape and other specialized items for skin, wound and ostomy care.
“It definitely appeals to my artistic side.”
“The dressings we use to protect a patient’s skin and support their healing can be quite detailed, with a variety of components that are put together step-by-step,” says Furtado, a skin, wound and ostomy nurse clinician at Hamilton Health Sciences (HHS). Dressings may also be custom-fit, depending on a patient’s needs.
“Putting together these dressings feels very much like artwork to me. It definitely appeals to my artistic side.”
Not your typical bandage
But assembling multi-piece dressings takes more than an artful hand. Some are highly complex, involving technology that keeps evolving. “I try to attend at least two conferences each year in order to stay caught up,” says Furtado.
“I enjoy complex dressings…”
A V.A.C. dressing, for example, comes in a kit that includes dressing foam, film seal, tubing and a vacuum pump. It’s used on complex wounds and pressure injuries.
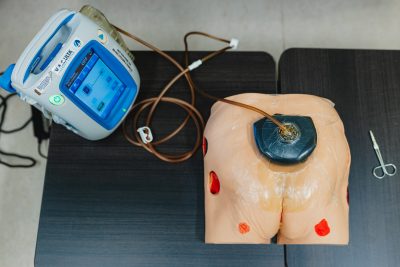
Some dressings, like this V.A.C. dressing, are highly complex and require a great deal of expertise to apply safely and correctly.
V.A.C. stands for vacuum-assisted closure, a method of decreasing air pressure around a wound to draw out fluid and infection to help with healing. To apply this dressing, Furtado places a foam bandage over an open wound, and a vacuum pump is used to help it heal faster.
“It literally pulls out drainage while pulling the wound together,” says Furtado. “We even have a version that cleans the wound with an antiseptic every couple of hours for infection prevention.”
Furtado demonstrates the expertise required to apply a V.A.C. dressing in this video:
Ostomy supplies are another example. They include barrier rings, flanges, powder and spray that layer together to protect skin surrounding a stoma – an abdominal opening made surgically when there are issues with the colon, so waste can be collected in a bag attached to the patient’s skin.
“We use our specialized knowledge and training to prevent the skin around the stoma from breaking down,” says Furtado, whose passion for skin, wound and ostomy care was ignited when she was a nursing student at McMaster.
Finding her passion
During a student placement with a home care agency, Furtado helped treat a case of flesh eating disease. “It was a very challenging wound, and treating this patient triggered my interest in wound care. I enjoy complex dressings, treating challenging wounds and seeing patients heal.”
“It takes a team to care for patients and help them recover.”
After graduating, Furtado worked at HHS Hamilton General Hospital’s burn unit for more exposure to wound care. Seven years later she switched to part-time in order to pursue specialty certification in wound, ostomy and continence care followed by a masters in wound healing from Western University. She then returned to HHS full time, splitting her time between McMaster Children’s Hospital and West Lincoln Memorial Hospital.
Other roles she has taken on due to her specialty include part-time assistant clinical professor at McMaster’s School of Nursing, faculty lecturer for the surgical foundations program at McMaster’s department of surgery, regional director for Nurses Specialized in Wound, Ostomy and Continence Canada (NSWOCC) as well as NSWOCC’s pediatric community of practice core program lead.
“The bottom line is, we don’t have fairy dust.”
At HHS, much of her work involves treating burns but she also sees a wide range of skin, wound and ostomy cases including pressure injuries.
“People can have serious complications if wounds aren’t cared for properly,” says Furtado. “In fact, it can be life threatening.”
Rosanne Zimmerman is HHS’ director of the patient experience and safety program, part of the quality and performance portfolio.
“Preventing hospital-acquired pressure injuries and sepsis are strategic priorities for HHS,” says Zimmerman. Pressure injuries are one source of infection that can lead to sepsis. HHS is also targeting surgical site infections, catheter-associated urinary tract infections and central line associated blood stream infections.
“I am incredibly proud of the work that Stephanie and the entire skin wound and ostomy team do every day in caring for our patients,” says Zimmerman.
It takes a team
Furtado credits HHS’ team approach with helping their patients recover. “With dressings, we’re trying to create the ideal circumstance for patients’ wounds to heal, but if they don’t have good blood flow to the area and good nutrition to build tissue it doesn’t matter what I do,” says Furtado, who works closely with staff members including other nurses, occupational therapists, physical therapists and dietitians.
“The bottom line is, we don’t have fairy dust. It takes a team to care for patients and help them recover.”



