
‘Silver lining’ lessons from COVID-19 pandemic
For two years, the COVID-19 pandemic has been a dark cloud hanging over the world. But every cloud has its silver lining.
At Hamilton Health Sciences (HHS), the pandemic sparked health-care advancements including the rapid expansion of virtual care, new collaborations and inventions, and made-in-Hamilton solutions to supply-chain issues that benefited both the hospital network and local businesses. Such innovations are expected to far outlive the pandemic.
Today marks two years since the World Health Organization declared the global COVID pandemic. Our organization grieves the losses brought by COVID and has lowered our flags to half-staff today. At the same time, HHS also recognizes key innovations and advancements that resulted from the experience and will stay with HHS long after the COVID storm cloud finally passes.
Virtual appointments
Prior to the pandemic, most out-patients visited the hospital in person for appointments with members of their health-care team. But a short appointment could easily balloon into a full-day commitment for patients travelling long distances. There were added expenses too, like gas, parking and meals.
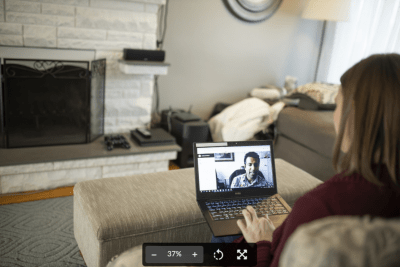
Many patients and physicians love the convenience of virtual appointments, where patients meet with their HHS health-care provider by phone or secure video conferencing.
With COVID outbreaks, and restrictions around entering hospital sites, the use of virtual appointments skyrocketed. Thousands of patients met with their health-care providers by phone or secure video conferencing. (Not every appointment is appropriate for virtual care, but often it makes sense).
The shift to remote care was swift. HHS had more virtual patient interactions in the month of April 2020 than in all of 2019. And one year into the pandemic, HHS had experienced a whopping 1,500 per cent increase in virtual care.

In one month alone, virtual visits saved HHS patients over 1.5 million kilometres of travel to and from hospital appointments.
Over 278,000 virtual visits took place at HHS clinics in 2021. Data showed that in one month alone, virtual visits saved HHS patients over 1.5 million kilometres of travel to and from appointments.
Lessons learned: Many patients and physicians love the convenience of virtual appointments. A 2021 HHS survey found that 85 per cent of patients were satisfied with virtual appointments and 98 per cent of the hospital network’s health-care providers wanted to continue with them as an option for meeting with patients.
Meanwhile, a 2021 Canada-wide survey by Canada Health Infoway found that 90 per cent of Canadians want technology that puts them in greater control of their health, while 80 per cent said they would use technology tools to help manage their health.
With the introduction of HHS’ new digital hospital information system this June, options like virtual visits, electronic referrals and e-consults will become established parts of the health-care system.
Post-surgical virtual care and remote home monitoring
Before the pandemic, most patients received follow-up care in person. For some, this meant longer hospital stays after surgery so they could be monitored by nurses, doctors and other health-care team members. For others, it meant leaving the comfort of home during their recovery to visit the hospital for follow-up care.
The Population Health Research Institute (PHRI), a joint research centre for HHS and McMaster University, had been testing virtual care and remote monitoring technology prior to COVID.
With virtual care and remote home monitoring, patients recover at home using technology such as tablet computers that connect them to HHS health-care providers. Patient information such as temperature, heart rate, and blood pressure is sent to health-care providers without requiring a trip to the hospital. Benefits include leaving the hospital sooner after surgery and avoiding trips to the emergency department once home. This also frees up beds and resources for other patients, which is expected to help reduce surgery backlog caused by COVID.
Lessons learned: Virtual care is here to stay. Investing in research and technology continues to be an important part of HHS’s vision to transform the way health care is provided.
New local supply chain partnerships
Prior to the pandemic, few people thought much about supply chains and how the flow of goods and services impacted their daily lives. The pandemic broke the global supply chain, making the sourcing of PPE and other critical supplies a serious challenge.

New HHS warehouse for personal protective equipment was established because of the pandemic.
Workplaces everywhere tried to get supplies from manufacturers that were either working as quickly as possible to keep up with demand or didn’t have raw materials from other areas of the world to make their product. In many cases, border and travel restrictions prevented products from entering the country.
As a result, new partnerships blossomed close to home and HHS established its own separate warehouse to store PPE as well as respiratory therapy items.
Lessons learned: HHS was contacted by a number of local companies that decided to retool or adapt their manufacturing operations to make PPE and other supplies for hospital use. It was a win-win. The decision to make hospital-grade PPE provided these businesses with the opportunity to keep workers employed and their plants operating, while helping their local hospital care for patients. Moving forward, HHS plans to leverage locally-manufactured products where possible, as well as ensuring that stock is rotated and products haven’t expired. HHS will also maintain its own pandemic warehouse.
New inventions
Necessity proved to be the mother of invention when a supply-chain shortage of small, plastic disposable forceps that work like tweezers threatened a busy virology lab’s ability to do COVID-19 tests.
The Hamilton Regional Laboratory Medicine Program’s (HRLMP) virology lab had been using the forceps for processing COVID-19 tests. Last fall, when the lab feared running out of forceps due to a global supply-chain shortage, lab staff together with the McMaster Manufacturing Research Institute (MMRI) and Coreprint Patterns, a precision mold-making and injection-molding firm in Hamilton, leapt into action to create an even better tool called a grasper.

The new grasper (right) was inspired by a supply chain shortage of pinchers (left).
Lessons learned: This collaboration, and new graspers, have been a huge success, and there’s no interest in going back to the old forceps.
When the going gets tough, HHS gets innovative
HHS has weathered a terrible two-year storm, and nimbly pivoted to keep its hospital sites running smoothly under extremely stressful conditions. Its health-care teams stood up to every new challenge, showing incredible resiliency in the face of adversity.
The pandemic continues to present significant challenges, driven most recently by the Omicron variant. Through it all, our teams have adapted and stayed solution-focused.
As 2022 continues to roll out, HHS remains cautiously optimistic for the year ahead – and eternally grateful for the dedication of its workforce.




